Translate this page into:
Cemented versus uncemented tibial components in primary total knee arthroplasty: A systematic review and meta-analysis of long-term outcomes
*Corresponding author: Zaki Al-Hifzi, Department of Arthroplasty and Musculoskeletal Oncology, King Faisal Medical City for Southern Region, Abha, Saudi Arabia. z_a_s1984@hotmail.com
-
Received: ,
Accepted: ,
How to cite this article: Al-Hifzi Z, Alshahrani BA, Al Athbah Y, Almoftery I. Cemented versus uncemented tibial components in primary total knee arthroplasty: A systematic review and meta-analysis of long-term outcomes. J Musculoskelet Surg Res. 2025;9:186-92. doi: 10.25259/JMSR_527_2024
Abstract
Uncemented total knee arthroplasty (TKA) is an emerging alternative to the traditional cemented TKA to improve biological ingrowth and reduce cement-related adverse effects. This study aimed to provide a comparative analysis of the cemented and uncemented tibial fixation for TKA. We searched PubMed, Embase, and Cochrane Library on April 15, 2024; after the extensive screening and risk of bias assessment, we extracted the relevant data and pooled the data as mean difference (MD) or odds ratio with a 95% confidence interval (CI). Ten randomized controlled trials were finally included in our meta-analysis. There was no significant difference between cemented and uncemented tibial components in terms of knee society score at 5 years (MD = −1.14, 95% CI [−3.77, 1.49], P = 0.39), range of motion (MD = 0.73, 95% CI [−2.47, 3.93], P = 0.65), flexion (MD = −1.23, 95% CI [−3.37, 0.92], P = 0.26), and extension (MD = 0.11, 95% CI [−0.21, 0.42], P = 0.51). However, there was a significantly greater maximum total point motion (MTPM) with uncemented fixation at 2 years (MD = −0.39, 95% CI [−0.68, −0.11], P = 0.007). Uncemented tibial fixation showed comparable outcomes to the cemented tibial fixation in TKA with significantly greater initial MTPM.
Keywords
Cemented fixation
Tibial component
Total knee arthroplasty
Uncemented fixation
INTRODUCTION
Knee osteoarthritis (OA) is a debilitating, degenerative joint disease characterized by progressive articular cartilage loss, synovitis, and bony remodeling, leading to significant pain and functional impairment.[1] Total knee arthroplasty (TKA) has emerged as a successful surgical intervention for end-stage knee OA, aiming to restore pain-free joint motion and improve quality of life.[2] A crucial aspect of TKA procedures is achieving durable implant fixation, which directly influences long-term outcomes and patient satisfaction.[3] Conventionally, cemented fixation with polymethylmethacrylate bone cement has been the gold standard for implant stability in TKA.[4] However, concerns regarding periprosthetic osteolysis, aseptic loosening, and potential stress shielding of bone due to the rigid cement interface have driven the development and exploration of cementless fixation techniques.[5]
Cementless fixation relies on biological ingrowth for implant stability, promoting bone apposition onto a porous implant surface. This theoretically offers advantages such as preservation of bone stock for potential future revision surgery, a more physiologic load transfer reducing stress shielding, and potentially improved long-term implant stability due to continuous bone remodeling.[6] The choice between cemented and cementless fixation in TKA remains a subject of ongoing debate. However, achieving initial implant stability and osseointegration can be a slower process with cementless techniques, potentially leading to increased micromotion and higher early aseptic loosening rates compared to cemented fixation.[7,8] Radiostereometric analysis (RSA) of new implants has been widely used to assess the risk of medium- to long-term failure due to aseptic loosening.[9] Implants showing continuous migration, i.e., more than 0.2 mm maximum total point motion (MTPM) in the 2nd year postoperatively, are considered at risk for aseptic loosening.[10,11]
Despite the growing body of literature comparing cemented and cementless fixation of tibial components in TKA, the evidence remains inconclusive. Existing studies often have small sample sizes, limited follow-up durations, and methodological heterogeneity, making it challenging to draw definitive conclusions about each technique’s comparative advantages and disadvantages. Therefore, this study aims to elucidate the comparative effectiveness of cemented versus uncemented tibial fixation in TKA.
MATERIALS AND METHODS
The study was conducted according to the preferred reporting items for systematic review and meta-analysis guidelines and checklist [Figure 1].[12] We also followed the rules of the Cochrane Handbook for Systematic Reviews of Interventions.[13]
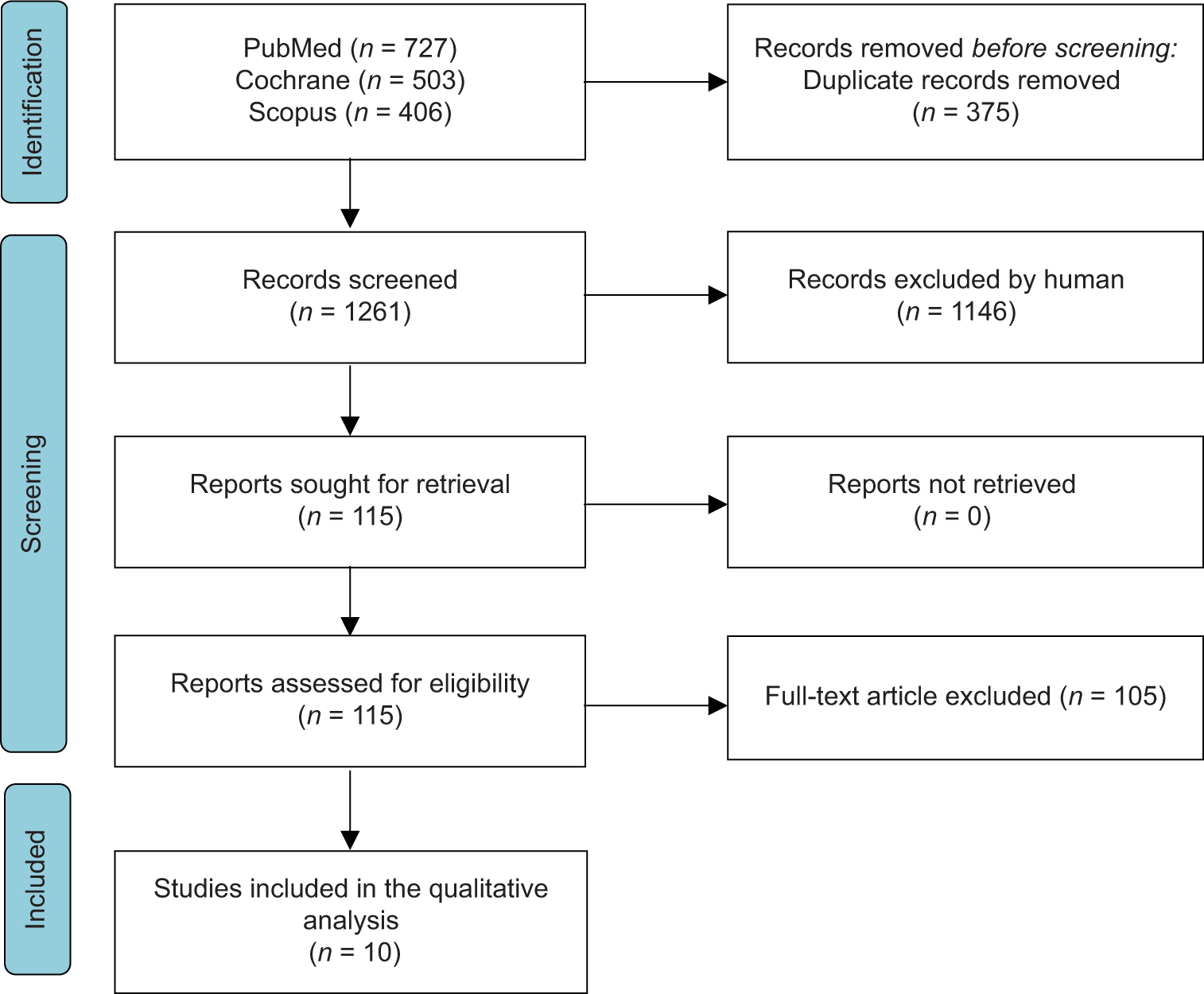
- Preferred reporting items for systematic review and meta-analysis follow-chart.
Literature search
We searched PubMed, Cochrane Library, and Scopus on June 15, 2024, for published randomized controlled trials using the following search strategy: ([(“Knee Replacement Arthroplasties”) OR (“Knee Replacement Arthroplasty”) OR (“Total Knee Replacement”) OR (“Total Knee Arthroplasty”)] AND [(“Uncemented” OR “uncement” OR “Cementless” OR “Non-cemented” OR Cemented OR cement*)]), also we manually screened the reference lists of the included studies for any eligible articles.
Eligibility criteria and study selection
We included randomized controlled trials that compared cemented and uncemented tibial component fixation in patients undergoing TKA. We excluded animal studies, cohort or case-control reports, in vitro studies, overlapped datasets, conference abstracts, reviews, book chapters, theses, editorial letters, and abstract-only papers. After duplicate removal using Endnote, two authors independently performed the title and abstract screening, then the full-text screening. Conflicts were solved by consulting a third author.
Data extraction
We extracted the patients’ baseline demographic characteristics, a summary of the main results of the included studies, and the following outcomes: Knee society score (KSS) at 5 years, range of motion (ROM), degree of flexion, degree of extension, and MTPM at 2 years.
Risk of bias assessment
Two authors independently assessed the quality of the included studies using the Cochrane risk of bias tool as described in the Cochrane Handbook.[14] The main assessed bias domains include selection bias, performance bias, detection bias, attrition bias, reporting bias, and other potential sources of bias.
Data synthesis
We used Review Manager software version 5.4 for the meta-analysis; continuous outcomes were pooled using main difference (MD), and dichotomous outcomes were pooled using odds ratio, all with 95% confidence intervals (CIs). Heterogeneity was assessed using chi-square and I-square tests. The studies were considered heterogeneous at chi-square P < 0.1 and I2 > 50%. A fixed effect model was used for the analysis unless heterogeneity was detected, in which case a random effect model was used.
RESULTS
We located 1636 articles through a literature search, and then after the title and abstract and full-text screening, 10 articles were finally included in the meta-analysis [Figure 1].[15-24]
Baseline characteristics of the included studies are shown in Table 1; they include age, sex, body mass index, and physical status. According to the authors’ judgment of the risk of bias, the overall quality of the included studies was moderate [Figure 2].
| Study ID | Sample size | Study group | Age (year) Mean (SD) | BMI (kg/m2) Mean (SD) | Sex, No. of females (%) | Physical status | ||
|---|---|---|---|---|---|---|---|---|
| ASA I n (%) | ASA II n (%) | ASA III n (%) | ||||||
| Nilsson et al., 2006[21] | 34 | Cemented | 55.5 (7.5) | 20 (59) | ||||
| 35 | Uncemented | 56 (6.25) | 23 (65) | |||||
| Wilson et al., 2012[23] | 18 | Cemented | 61 (9) | 34 (5) | 10 (56) | |||
| 27 | Uncemented | 60 (8) | 32 (5) | 17 (63) | ||||
| Fernandez-Fairen et al. 2013[16] | 63 | Cemented | 60 (4.6) | 30.5 (4.90) | 54 (76) | |||
| 69 | Uncemented | 61 (5.0) | 29.1 (5.2) | 55 (74) | ||||
| Choy et al., 2014[15] | 86 | Cemented | 69 (6.8) | 29 (4) | 62 (72) | |||
| 82 | Uncemented | 65 (5) | 30 (6) | 60 (73) | ||||
| Pulido et al., 2015[20] | 126 | Cemented | 68.4 (8.3) | 31.8 (6.5) | 71 (56) | |||
| 106 | Uncemented | 68.1 (8.8) | 31.4 (6.3) | 51 (48) | ||||
| Van Hamersveld et al., 2017[24] | 30 | Cemented | 65.7 (6.3) | 28.6 (3.6) | 13 (43.3) | 8 (26.7) | 20 (66.7) | 2 (6.7) |
| 30 | Uncemented | 66.8 (9.1) | 28.0 (3.3) | 19 (63.3) | 5 (16.7) | 18 (60) | 7 (23.3) | |
| Hampton et al., 2020[17] | 45 | Cemented | 63 (3.5) | 30.7 (3.25) | 23 (51.1) | |||
| 45 | Uncemented | 64 (5) | 30.1 (3.5) | 25 (44.4) | ||||
| Nivbrant et al., 2020[22] | 51 | Cemented | 67.8 (8.0) | 30.9 (4.6) | ||||
| 49 | Uncemented | 68.8 (7.5) | 30.3 (5.1) | |||||
| van der Lelij et al., 2023[19] | 34 | Cemented | 66 (6.3) | 30 (3.1) | 16 (47) | 4 (12) | 26 (77) | 4 (12) |
| 35 | Uncemented | 65 (5.7) | 28 (3.1) | 17 (49) | 13 (37) | 21 (60) | 1 (3) | |
| Gibon et al., 2023[18] | 135 | Cemented | 68 | 32 | 77 (57) | |||
| 126 | Uncemented | 68 | 31 | 60 (48) | ||||
ASA: American Society of Anesthesiologists, BMI: Body mass index, SD: Standard deviation

- Risk of bias assessment for included studies. Green circles with plus sign: Low risk of bias. Yellow circles with question mark: Unclear risk of bias.
Meta-analysis results
KSS at 5 years
The outcome was reported in five studies with 565 total patients, the pooled mean difference (MD) showed no statistically significant difference between the cemented and uncemented tibial fixation in KSS score at 5 years (MD = −1.14, 95% CI [−3.77, 1.49], P = 0.39), the pooled results were heterogeneous (P = 0.09, I2 = 50%), the heterogeneity was best solved by removing Fernandez-Fairen et al. 2013[16] (P = 0.50, I2 = 0%), and the MD remained non-significant (P = 0.76) [Figure 3].
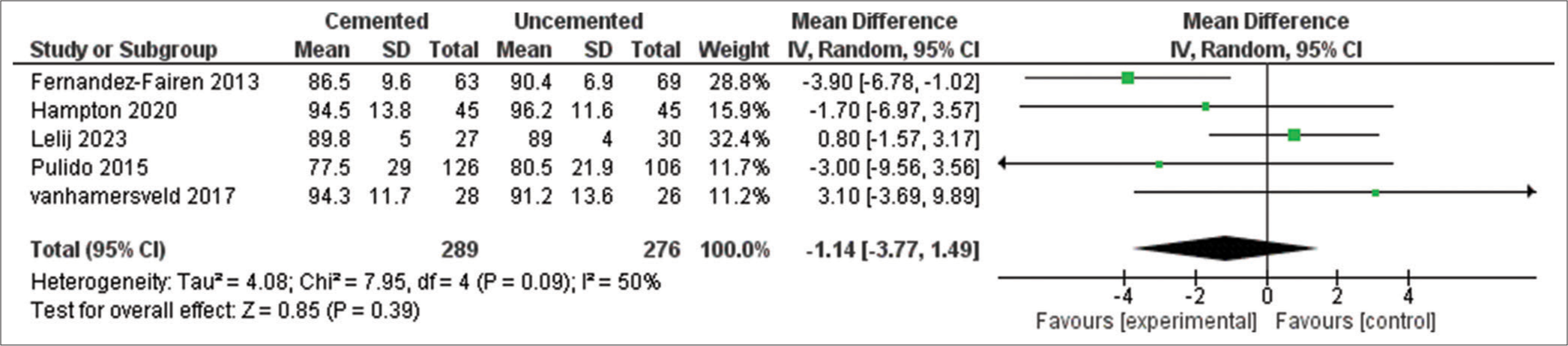
- Knee society score at 5 years. SD: Standard deviation, CI: Confidence interval, IV: Inverse variance, df: Degree of freedom, Tau2: Between-study variance, Chi2: Chi-square test for heterogeneity, I2: Inconsistency statistics (heterogeneity), Z: Z-score for overall effect, P: P-value for statistical significance.
MTPM at 2 years
The outcome was reported in four studies with 232 total patients. It was measured by RSA [Figure 4]. The pooled result showed significantly higher MTPM with uncemented tibial fixation (MD = −0.39, 95%CI [−0.68, −0.11], P = 0.007), the results were heterogeneous (P = 0.007, I2 = 75%), the heterogeneity was solved by removal of Nivbrant et al. 2020[22] (P = 0.33, I2 = 11%). The effect estimate remained significant (P < 0.0001).
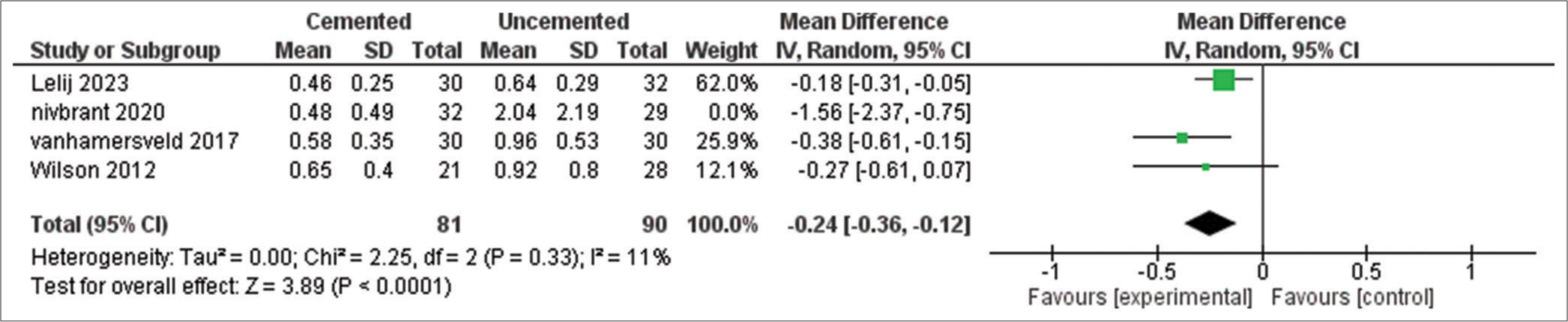
- Maximum total point motion at 2 years. SD: Standard deviation, CI: Confidence interval, IV: Inverse variance, df: Degree of freedom, Tau2: Between-study variance, Chi2: Chi-square test for heterogeneity, I2: Inconsistency statistics (heterogeneity), Z: Z-score for overall effect, P: P-value for statistical significance.
ROM (in degrees)
The outcome was reported in two studies with 237 patients [Figure 5]. The pooled MD showed no significant difference between cemented and uncemented tibial fixation in postoperative ROM (MD = 0.73, 95%CI [−2.47, 3.93], P = 0.65), and the pooled results were homogeneous (P = 0.91, I2 = 0%).
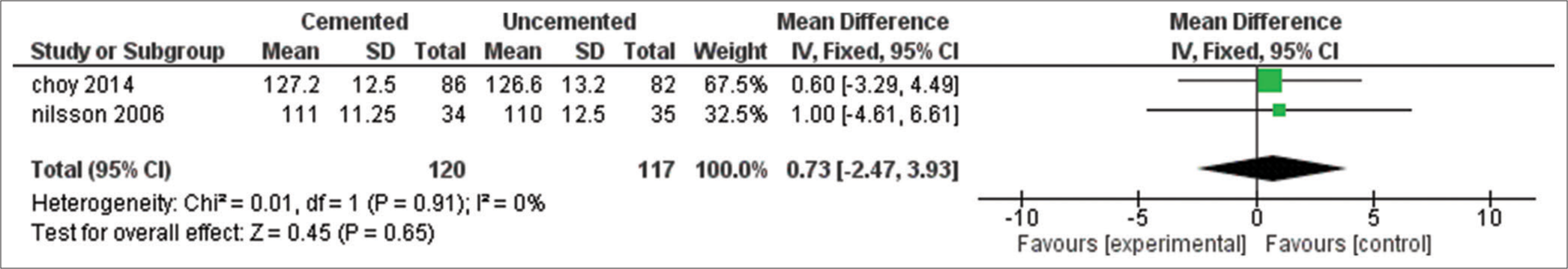
- Range of motion (in degrees). SD: Standard deviation, CI: Confidence interval, IV: Inverse variance, df: Degree of freedom, Tau2: Between-study variance, Chi2: Chi-square test for heterogeneity, I2: Inconsistency statistics (heterogeneity), Z: Z-score for overall effect, P: P-value for statistical significance.
Motion flexion (degrees)
The outcome was reported in three studies with 547 patients [Figure 6]. The pooled MD showed no significant difference between cemented and uncemented tibial fixation in postoperative motion flexion (MD = −1.23, 95%CI [−3.37, 0.92], P = 0.26), and the pooled results were homogeneous (P = 0.12, I2 = 52%).
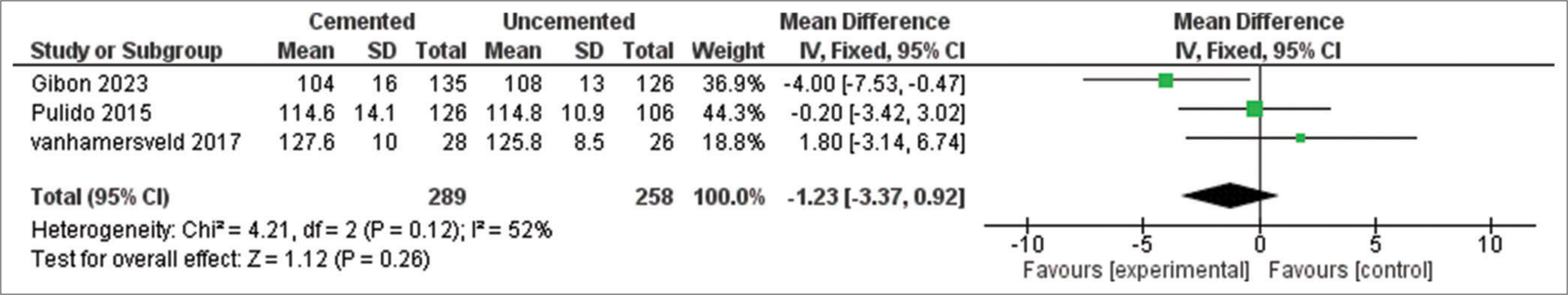
- Motion flexion (degrees). SD: Standard deviation, CI: Confidence interval, IV: Inverse variance, df: Degree of freedom, Tau2: Between-study variance, Chi2: Chi-square test for heterogeneity, I2: Inconsistency statistics (heterogeneity), Z: Z-score for overall effect, P: P-value for statistical significance.
Motion extension (degrees)
Three studies reported the outcome with 547 patients [Figure 7]. The pooled MD showed no significant difference between cemented and uncemented tibial fixation in postoperative motion extension (MD = 0.11, 95%CI [−0.21, 0.42], P = 0.51), and the pooled results were homogeneous (P = 0.23, I2 = 31%).
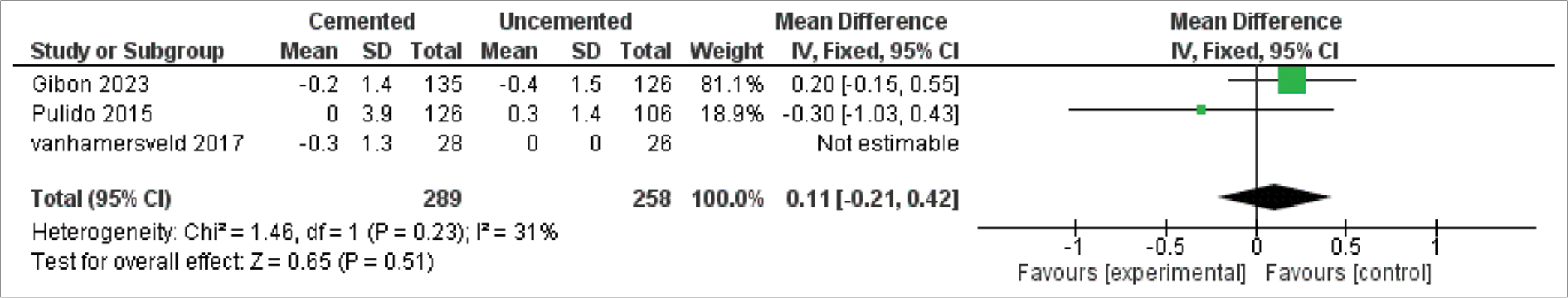
- Motion extension (degrees). SD: Standard deviation, CI: Confidence interval, IV: Inverse variance, df: Degree of freedom, Tau2: Between-study variance, Chi2: Chi-square test for heterogeneity, I2: Inconsistency statistics (heterogeneity), Z: Z-score for overall effect, P: P-value for statistical significance.
DISCUSSION
Cemented designs were widely preferred for TKA. However, an uncemented fixation design was developed due to the increased aseptic loosening and loss of cement-bone interlock due to trabecular resorption along with the deformation and degradation of the cement mantle.[25,26] Uncemented TKA was thought to provide strong long-term biological fixation due to bone ingrowth.[27] Several biomaterials have been used to enhance bone ingrowth in uncemented TKA, like osteoconductive hydroxyapatite (HA) coatings, peri-apatite (PA) HA, and trabecular metal.[23,28,29] Several factors have been linked to TKA failure, one of which is the lack of fixation of the implant, especially on the tibial side, particularly in patients younger than 65 years.[30,31] This systematic review and meta-analysis compared the functional and radiological outcomes of cemented and uncemented tibial components for primary TKA.
Our results showed no significant difference between cemented and uncemented tibial fixation in a 5-year follow-up duration. This is similar to the results reported by the previous meta-analysis, which showed no significant difference between cementless porous tantalum tibial components and the traditional cemented tibial components in primary TKA.[32] The outcome was reported by five studies; three of them used porous tantalum for the uncemented tibial component,[16,17,20] van der Lelij et al. used 3D-printed Triathlon Tritanium (Stryker) cruciate retaining, and Van Hamersveld et al. used PA coating for the uncemented fixation.[19,24] Regardless of the different biomaterials used for uncemented tibial fixation, the studies individually reported no significant difference in KSS score at 5 years. However, at 11–15-year follow-up, Hampton et al. showed significantly better KSS scores with uncemented tibial fixation,[17] which was different from the results reported by Choy et al. and Li et al.[15,32]
Our results showed significantly higher MTPM with uncemented tibial fixation. Four included studies reported the outcome. Van der Lelij et al., Nivbrant et al. and Van Hamersveld et al. showed significantly higher MTPM with uncemented fixation at 2 years. However, Wilson et al. reported no significant difference between cemented and uncemented tibial fixation at 2 years.[19,22-24] This is similar to the results reported by the previous meta-analysis by Fozo et al. comparing cemented, uncemented, and hybrid techniques for both tibial and femoral components.[33] Both excessive initial migration in the 1st year and high continuous migration after 1 year are used to determine implant fixation and longevity.[9,34] However, regardless of the initial migration, highly porous and HA-coated uncemented components were found firmly fixed to the bone at long-term follow-up.[35,36] Thus, more long-term clinical trials are needed to assess the long-term stability of the uncemented tibial fixation.
One of the primary goals of TKA is pain relief and ROM restoration.[37] Moreover, knee flexion ROM after TKA is significantly associated with acute postoperative ROM.[38] Our analysis showed no significant difference in ROM, flexion, or extension between cemented and uncemented tibial components in TKA. Similar results were also reported in the previous meta-analysis.[32]
Our study provides a comprehensive overview of the outcomes of cemented and uncemented tibial components for TKA. However, notable heterogeneity was encountered in the main outcomes. Moreover, the mean duration of follow-up was relatively short, and more studies are needed to provide the long-term stability results for the uncemented tibial fixation.
CONCLUSION
Uncemented tibial fixation for TKA warrants a remarkable instability as it showed significantly greater MPTM compared to the traditional cemented fixation at 2 years. However, uncemented and cemented fixations were comparable to the other assessed outcomes.
Authors’ contributions
ZA: Conceptualization, supervision, validation. YA: Writing – review and editing, supervision, validation. IA and BA: Writing – original draft preparation, data curation, visualization, and methodology. All authors have critically reviewed and approved the final draft and are responsible for the manuscript’s content and similarity index.
Ethical approval
Institutional Review Board approval is not required.
Declaration of patient consent
Patient consent is not required, as there are no patients in this study.
Use of artificial intelligence (AI)-assisted technology for manuscript preparation
The authors confirm that there was no use of artificial intelligence (AI)-assisted technology for assisting in the writing or editing of the manuscript and no images were manipulated using AI.
Conflicts of interest
There are no conflicting relationships or activities.
Financial support and sponsorship: This study did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
References
- Recent advances in the treatment of osteoarthritis. F1000Res. 2020;9:325.
- [CrossRef] [PubMed] [Google Scholar]
- New technologies in knee arthroplasty: Current concepts. J Clin Med. 2020;10:47.
- [CrossRef] [PubMed] [Google Scholar]
- Patient relevant outcomes of unicompartmental versus total knee replacement: Systematic review and meta-analysis. BMJ. 2019;364:l352.
- [CrossRef] [PubMed] [Google Scholar]
- Cemented vs. cementless fixation in primary knee replacement: A narrative review. Materials (Basel). 2024;17:1136.
- [CrossRef] [PubMed] [Google Scholar]
- Periprosthetic bone loss: Diagnostic and therapeutic approaches. F1000Res. 2014;2:266.
- [CrossRef] [PubMed] [Google Scholar]
- Biomechanical behaviours of the bone-implant interface: A review. J R Soc Interface. 2019;16:20190259.
- [CrossRef] [PubMed] [Google Scholar]
- New horizons of cementless total knee arthroplasty. J Clin Med. 2024;13:233.
- [CrossRef] [PubMed] [Google Scholar]
- Unicompartmental knee arthroplasty, an enigma, and the ten enigmas of medial UKA. J Orthop Traumatol. 2020;21:15.
- [CrossRef] [PubMed] [Google Scholar]
- RSA and registries: The quest for phased introduction of new implants. J Bone Joint Surg Am. 2011;93(Suppl 3):62-5.
- [CrossRef] [PubMed] [Google Scholar]
- Roentgen stereophotogrammetric analysis as a predictor of mechanical loosening of knee prostheses. J Bone Joint Surg [Br]. 1995;77-B:377-83.
- [CrossRef] [Google Scholar]
- Fixation of a trabecular metal knee arthroplasty component. A prospective randomized study. J Bone Joint Surg Am. 2009;91:1578-86.
- [CrossRef] [PubMed] [Google Scholar]
- The PRISMA 2020 statement: An updated guideline for reporting systematic reviews. BMJ. 2021;372:n71.
- [CrossRef] [PubMed] [Google Scholar]
- Updated guidance for trusted systematic reviews: A new edition of the Cochrane Handbook for Systematic Reviews of Interventions. Cochrane Database Syst Rev. 2019;10:ED000142.
- [CrossRef] [PubMed] [Google Scholar]
- Cochrane handbook for systematic reviews of interventions In: Higgins JP, Green S, eds. Cochrane book series. Chichester, UK: John Wiley and Sons, Ltd; 2008. p. :1-649.
- [CrossRef] [Google Scholar]
- Cemented versus cementless fixation of a tibial component in LCS mobile-bearing total knee arthroplasty performed by a single surgeon. J Arthroplasty. 2014;29:2397-401.
- [CrossRef] [PubMed] [Google Scholar]
- Trabecular metal in total knee arthroplasty associated with higher knee scores: A randomized controlled trial. Clin Orthop Relat Res. 2013;471:3543-53.
- [CrossRef] [PubMed] [Google Scholar]
- Uncemented tantalum metal components versus cemented tibial components in total knee arthroplasty: 11-to 15-year outcomes of a single-blinded randomized controlled trial. Bone Joint J. 2020;102:1025-32.
- [CrossRef] [PubMed] [Google Scholar]
- Randomized clinical trial of cementless versus cemented tibial components: Durable and reliable at a mean 10-years follow-up. J Arthroplasty. 2023;38:S14-20.
- [CrossRef] [PubMed] [Google Scholar]
- Continued stabilization of a cementless 3D-printed total knee arthroplasty: Five-year results of a randomized controlled trial using radiostereometric analysis. J Bone Joint Surg Am. 2023;105:1686-94.
- [CrossRef] [PubMed] [Google Scholar]
- The Mark Coventry award: Trabecular metal tibial components were durable and reliable in primary total knee arthroplasty: A randomized clinical trial. Clin Orthop Relat Res. 2015;473:34-42.
- [CrossRef] [PubMed] [Google Scholar]
- Uncemented HA-coated implant is the optimum fixation for TKA in the young patient. Clin Orthop Relat Res. 2006;448:129-39.
- [CrossRef] [PubMed] [Google Scholar]
- Cementless versus cemented tibial fixation in posterior stabilized total knee replacement: A randomized trial. J Bone Joint Surg Am. 2020;102:1075-82.
- [CrossRef] [PubMed] [Google Scholar]
- Continued stabilization of trabecular metal tibial monoblock total knee arthroplasty components at 5 years-measured with radiostereometric analysis. Acta Orthop. 2012;83:36-40.
- [CrossRef] [PubMed] [Google Scholar]
- Fixation and clinical outcome of uncemented peri-apatite-coated versus cemented total knee arthroplasty: Five-year follow-up of a randomized controlled trial using radiostereometric analysis (RSA) Bone Joint J. 2017;99B:1467-76.
- [CrossRef] [PubMed] [Google Scholar]
- Fixation for primary total knee arthroplasty: Cemented. J Arthroplasty. 1996;11:123-5.
- [CrossRef] [PubMed] [Google Scholar]
- The scientific basis of cement versus cementless fixation. Clin Orthop Relat Res. 1992;276:19-25.
- [CrossRef] [Google Scholar]
- Cementless total knee arthroplasty in patients 50 years or younger. Clin Orthop Relat Res. 2002;404:102-27.
- [CrossRef] [PubMed] [Google Scholar]
- Osteoconductive coatings for total joint arthroplasty. Clin Orthop Relat Res. 2002;395:53-65.
- [CrossRef] [PubMed] [Google Scholar]
- Hydroxyapatite: from plasma spray to electrochemical deposition In: Epinette J, Manley MT, eds. Fifteen years of clinical experience with hydroxyapatite coatings in joint arthroplasty. Paris: Springer; 2004. p. :29-33.
- [CrossRef] [Google Scholar]
- Higher cumulative revision rate of knee arthroplasties in younger patients with osteoarthritis. Clin Orthop Relat Res. 2004;421:162-8.
- [CrossRef] [PubMed] [Google Scholar]
- The Swedish knee arthroplasty register 1975-1997: An update with special emphasis on 41,223 knees operated on in 1988-1997. Acta Orthop Scand. 2001;72:503-13.
- [CrossRef] [PubMed] [Google Scholar]
- Efficacy of cementless porous tantalum tibial components versus cemented tibial components in primary total knee arthroplasty: A meta-analysis. Medicine (Baltimore). 2024;103:e37697.
- [CrossRef] [PubMed] [Google Scholar]
- A Systematic review and network meta-analysis of the outcomes of patients with total knee arthroplasty using cemented, uncemented, or hybrid techniques. Cureus. 2023;15:e47299.
- [CrossRef] [Google Scholar]
- Early migration of tibial components is associated with late revision: A systematic review and meta-analysis of 21,000 knee arthroplasties. Acta Orthop. 2012;83:614-24.
- [CrossRef] [PubMed] [Google Scholar]
- Trabecular metal tibial knee component still stable at 10 years. Acta Orthop. 2016;87:504-10.
- [CrossRef] [PubMed] [Google Scholar]
- The beneficial effect of hydroxyapatite lasts: A randomized radiostereometric trial comparing hydroxyapatite-coated, uncoated, and cemented tibial components for up to 16 years. Acta Orthop. 2012;83:135-41.
- [CrossRef] [PubMed] [Google Scholar]
- Increased range of motion is important for functional outcome and satisfaction after total knee arthroplasty in Asian patients. J Arthroplasty. 2016;6:1199-203.
- [CrossRef] [PubMed] [Google Scholar]
- Is discharge knee range of motion a useful and relevant clinical indicator after total knee replacement? Part 2. J Eval Clin Pract. 2012;3:652-8.
- [CrossRef] [PubMed] [Google Scholar]






