Translate this page into:
Factors affecting the outcome in the correction of angular deformities around the knee using extraperiosteal tension band plate: A local experience
Corresponding Author:
Munzir I. A. Gaboura
Department of Reconstructive Orthopaedics, Division of Paediatric Orthopaedic, King Fahad Medical City, PO Box: 59046, Riyadh 11525
Saudi Arabia
munzirgaboura@gmail.com
| How to cite this article: Gaboura MI, Kazi K, Abak AA, AlRumaih M, AlKenani A. Factors affecting the outcome in the correction of angular deformities around the knee using extraperiosteal tension band plate: A local experience. J Musculoskelet Surg Res 2020;4:146-151 |
Abstract
Objectives: The aim of this study is to reflect on our local experience with extraperiosteal tension band plate around the knee and the factors that affect the outcome. Methods: This is a retrospective review of 21 patients (34 limbs) and involving 35 segments gathered and treated during a period from 2007 to 2018 by a single surgeon employing a standardized technique. The inclusion criteria were all patients with coronal plane deformities around the knee with an open physis, regardless of pathological background. Patients who had previous or concurrent surgeries for the same problem were excluded from the study. Patients' age and body mass index were recorded. Mechanical axis deviation (MAD) distance, tibio-femoral (T-F) angle, mechanical lateral distal femoral angle, and mechanical medial proximal tibia angle were measured from a standing anteroposterior radiograph. Results: The average age was 6.5 years, and the mean duration of treatment was 13.6 months, with “sick physis” requiring longer durations. The mean rate of correction of T-F angle was 1.5°/month. The MAD distance improved at an average rate of 2.4 mm/month. The distal femur physis improved at a rate of 0.69°/month, while the proximal tibia physis improved at a rate of 0.58°/month. Conclusion: The severity of preoperative deformity influenced the rate of correction, and this is further influenced by the pathological background and physis treated, femora faster than tibiae. Patients with more than 3 years of growth remaining showed faster correction.
Introduction
Hemiepiphysiodesis in treating knee deformities in children has evolved over the years. Available options are either open or percutaneous and either temporary or permanent with various techniques and implants.[1],[2],[3],[4]
Hemiepiphyseal stapling technique by Blount and Clarke[5],[6] and percutaneous transphyseal screw technique by Métaizeau et al.[7],[8] have all been in wide practice. Concerns such as metal back-out and premature physeal arrest in addition to inadvertent overcorrection and under-correction led to wean off from Blount and Clarke technique over the past two decades. The downside of Métaizeau et al.'s technique could be the postulated compression effect on the physis providing a slow correction.
The tension band plate (TBP) concept since the advent by Stevens[9] has been a standard approach by most surgeons.[10],[11],[12] The ease of application and the excellent results to date have led to the widespread use. The TBP applied at the periphery of the growth plate acts as a hinge allowing divergence of screws as the growth progress, and as the bending moment increases, the plate itself bends, preventing compression and hence decreasing the risk of local growth plate tethering. Many researchers concluded that the concept of osteotomy as a first resort and criterion standard has become outdated.[9],[11],[12]
This study aims to assess the efficacy of the TBP and the parameters that influence the outcome in angular deformity correction.
Materials and Methods
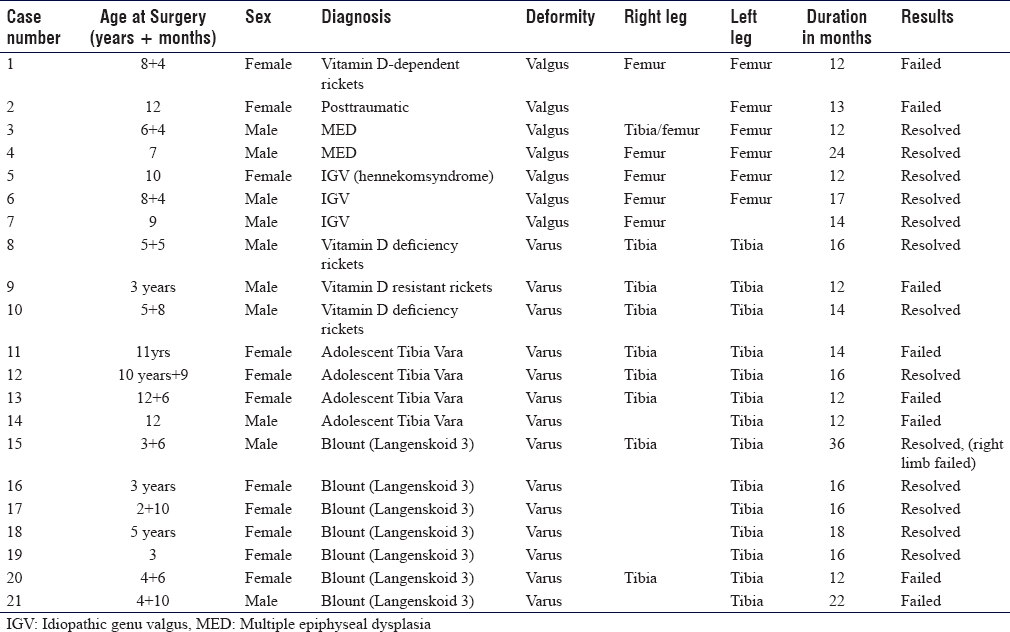
With prior institutional review board approval and in a retrospective manner, a total of 36 patients were found, of which 21 patients (34 limbs) were included in the study. The inclusion criteria were all patients with coronal plane deformities around the knee with an open physis, regardless of pathological background. Patients with previous surgical intervention or concurrent knee procedures were excluded. The patients were gathered and treated from 2007 to 2018 by a single surgeon employing a standardized technique, with an extraperiosteal TBP and two nonlocking screws instead of stapling or transphyseal screws. The age distribution, etiology, and location of the deformities and outcomes are depicted in [Table - 1].
The preoperative assessment included measurement of limb length and gait assessment specifically for varus thrust, and the clinical assessment of the deformity, including rotational and sagittal plane deformities as well as patella tracking, and ligamentous laxity was noted as well.
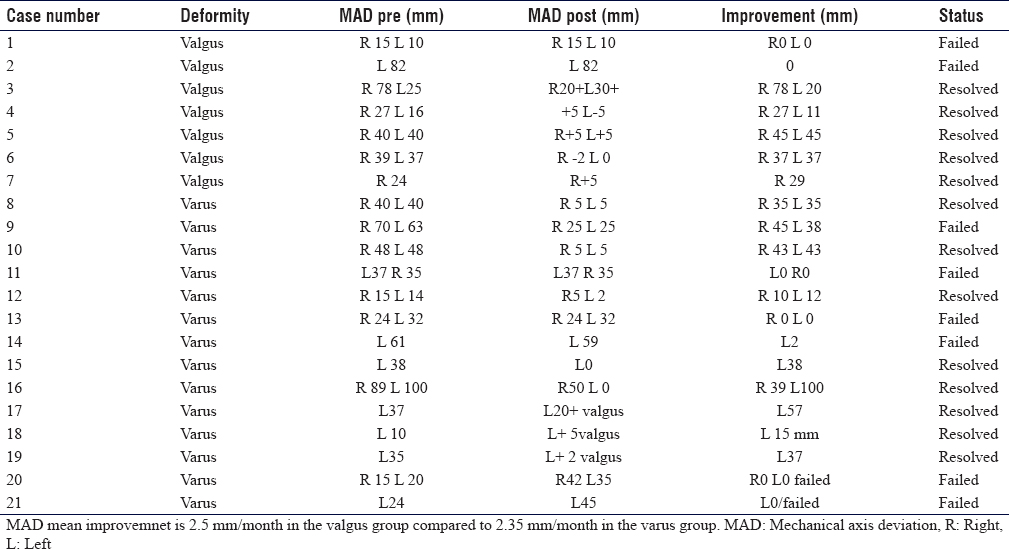
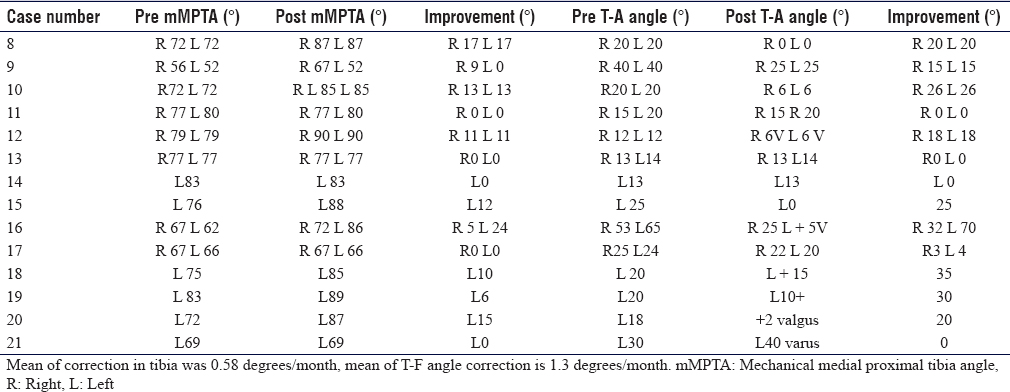
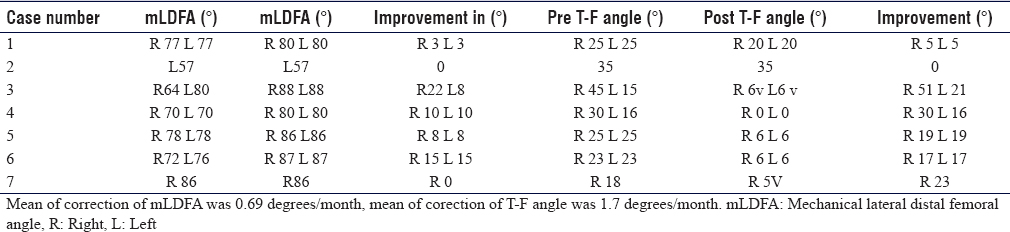
Radiographic assessment included a long-standing anteroposterior (AP) radiograph with the patella facing forward was requested for all patients, and lateral views at the knee and patella if deemed necessary. The mechanical axis deviation (MAD) distance, mechanical lateral distal femoral angle (mLDFA), tibio-femoral (T-F) angle, and mechanical medial proximal tibial angle (mMPTA) were recorded for each deformity [Figure - 1], [Figure - 2] and [Table - 2], [Table - 3], [Table - 4].[13]
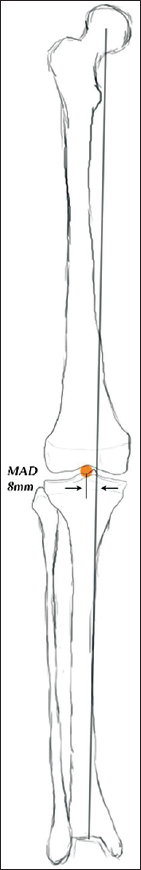 |
| Figure 1: A drawing showing the mechanical axis deviation distance. Normal is 8 mm |
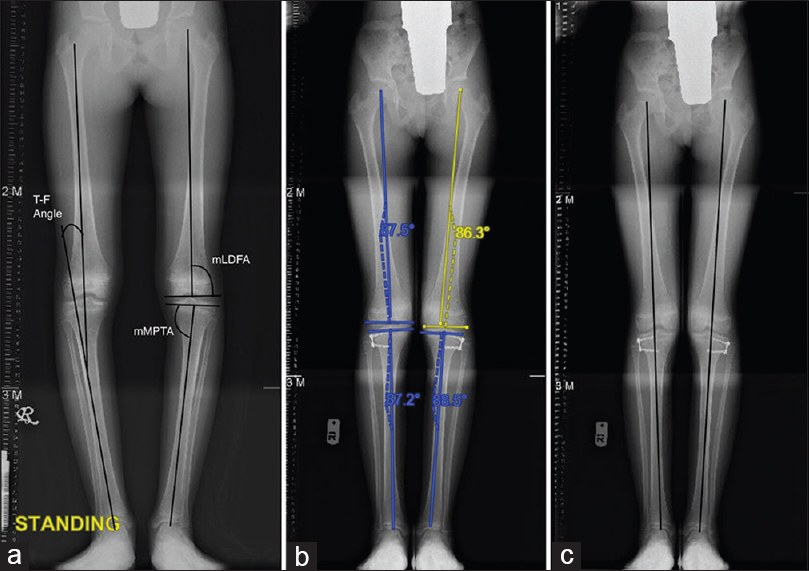 |
| Figure 2: A 12-year-old girl case of bilateral adolescent tibia vara (a) mechanical lateral distal femoral angle, mechanical medial proximal tibial angle, tibio-femoral angle (b) 12 months postcorrection, note the screw divergence to about 40 degrees (c) normal mechanical axis within the inner two zones |
Cases with severe apparent deformity were offered surgery, those with mild deformity were offered observation for a period of 6–12 months, and if their deformity progressed, surgery was indicated.
The radiological indication was a mechanical axis lying outside the inner two zones of six-zone division knee (three medial and three lateral) [Figure - 3].[12]
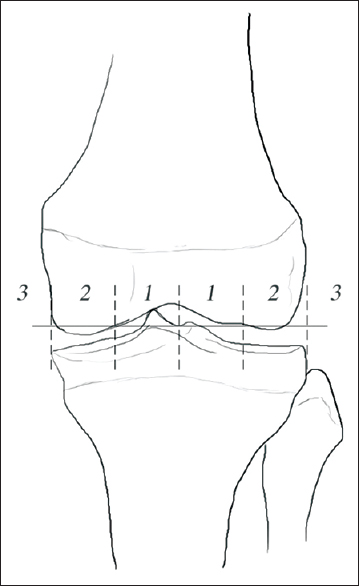 |
| Figure 3: A drawing illustrates the six zones of the knee. Surgical indication is deemed necessary when the mechanical axis fall outside the inner two zones. As this has been reflected in affecting the ground reaction forces |
Hand bone age was deemed necessary for patients approaching maturity to assess the potential for growth. Our age reference for maturity was 14 in females and 16 in males.
The surgical procedure was done as a day case basis through the pediatric daycare unit under general anesthesia. The surgical time ranged from 30 to 60 min.
The desired correction was the restoration of the mechanical axis within the inner two zones of a six-zone division of an AP radiograph of the knee; when this occurs, there will be an improvement in the position of the ground reaction forces [Figure - 3].[13],[14]
Results
The endpoint for the procedure was to reach a neutral mechanical axis within the inner two zones of a six-zone knee as described [Figure - 3]; failed cases are those that did not achieve that or failed to show good progression during an expected time frame (12–24 months) or needed an osteotomy as such.
Overall, there were 21 cases of which 13 resolved (22 segments), while 8 cases failed (11 segments) to achieve normalized mechanical axis. There were 11 females and 10 males; there were 13 bilateral and 8 unilateral cases. The mean age was 6.5 years (3–12.6 years) and weight ranged from 15 kg unto 91 kg.
The preoperative deformity ranged from 65° varus to 45° valgus, the mean deformity for genu varus was 23.1°, and the mean deformity for genu valgus was 28.7°. The MAD distance[13] was recorded [Figure - 1], which is a good reflection of correction as well as the effect it has on hip and ankle biomechanics.[14] The MAD ranged from 100 mm varus to 75 mm valgus. The preoperative mLDFA ranged from 57° to 86°, and the mMPTA ranged between 56° and 83°.
The mean duration of implantation was 13.6 months in the range of 12–24 months. This is probably reflected back to the wide range and diversity of the deformities and the wide scope of underlying pathology. There was a mean rate of correction of 0.69° (0.25°–1.8°)/month in the distal femur and 0.58° (0.4°–1.4°)/month in the proximal tibia. The mean improvement of the MAD in the varus cases was 2.35 mm/month and in the valgus group was 2.5 mm/month. During the implantation period, the mean rate of correction of T-F angle was 1.5°/month.
Overall, all patients maintained adequate sagittal balance and the adequate horizontal plane of the axis during the implantation period. No element of leg length discrepancy was noted or iatrogenic premature physeal arrest. All wounds healed nicely without either superficial or deep infection noted. Furthermore, all patients were fully ambulant and pain-free, usually within 1–2 weeks after surgery.
Follow-up was planned at 3, 6, and another 6 months, depending on how fast the deformity was improving.
Discussion
In this study, all cases of genu valgus resolved with good correction. One patient had a rebound phenomenon (2 femurs) after 2 years from implant removal. A case of traumatic genu valgus was resistant, requiring a distal femur corrective osteotomy at a later age. Our series revealed satisfactory outcomes in cases of infantile Blount's (Langenskiold II–III).[15] The rate of correction was much influenced by the physis treated and the child's age and more or less to the weight of the patient in certain cases, such as infantile or adolescent Blount's.[16] Out of the seven cases, five completely resolved and two cases failed. The failed cases were quite obvious that were related to high body mass index (BMI) (about 43 kg/m2).[16] Furthermore, the presence of lateral thrust during gait implying a lax lateral collateral ligament. It was generally observed that the time to the correction of the neutral mechanical axis was longer. One case of Blount's disease required three consequent repetitive surgeries to normalize the mechanical axis. Cases of Vitamin D deficiency were four cases; two of them resolved and two failed. Those failed recalcitrant cases were Vitamin D-dependent rickets Type 1 and Vitamin D-resistant rickets with extensive deformity and poor bone quality.
With regard to adolescent tibia vara [Figure - 2], the correction was very limited, and only one of the four cases resolved. Many authors have explained failures as a result of the age of the patient and the fact that there was not enough growth potential left for guided growth. Chronological age is a controversial parameter, as is bone age, which is based on the Greulich and Pyle Radiographic Atlas of Skeletal Development. However, most of them had an open physis, and it was cross-checked with hands bone age.
From a complication perspective, an event of a broken screw (4.5 mm) was encountered in a case of infantile Blount's; the patient had a BMI of 43 kg/m2. Another case scenario was screw migration in a patient with Vitamin D-resistant rickets. It could be due to the surgical technique as the result of the distal screw was not well engaged in the epiphysis and was quite close to the growth plate; during follow-up, the whole system was found to be migrated to the metaphysis. Such a scenario was also reported in a study by Ballal et al.[12]
We have noted that in our Blount's cases, the Langenskiold stage,[15] BMI, and the presence of the lateral thrust decreased the efficacy of the TBP; moreover, the duration was longer. One of the patients needed three surgeries of TBP exchanges as it reached the maximum limit, and the patient was still having sufficient potential for growth.
Schroerlucke et al. showed a high rate of implant failure with TBP in the series with 18 Blount's disease patients, with eight hardware failures, mostly postulated due to high BMI. In our study, we had seven Blount's cases, of which two cases failed to correct; it was directly proportional to the very high BMI and presence of the lateral thrust, which concurs Schroerlucke et al.'s observations.[16]
We cannot completely conclude that TBP should not be used in “sick physis.” This term reflects sickness because of gravity, eccentric loading, and ligament laxity, compounded by associated shear and torsional forces.[9],[17] However, parents should be informed about the risks of needing multiple surgeries, failures, and longer durations to attain correction. Cases of nutritional rickets correct dramatically, but recalcitrant cases probably reflect the intense metabolic background, such as in our cases, Vitamin D-dependent and -resistant rickets.
In our study, we had observed limited use of TBP with adolescent tibia vara. McIntosh et al.[18] concluded in their study that lateral hemiepiphysiodesis for the treatment of adolescent tibia vara should be reserved for younger patients <14 years with mild preoperative varus deformity and BMI <45 kg/m2.
Generally, genu valgum had a better and faster correction than genu varus, which was evident in our study. The causes of this need to be further addressed; speculations such that the femur has more contribution to the overall general limb length has been put forward.[19] In addition to this, we had two cases of genu valgum with an underlying multiple epiphyseal dysplasia, who had excellent outcomes.
The limitations of this study are reflected in the small number of patients and its retrospective design.
Conclusion
Hemiepiphysiodesis with TBP still stands to be a valid procedure for coronal plane deformities correction around the knee. Adequate patient selection is needed for better outcome. This implies noting the pathological background, “healthy physis” being faster to correct than “sick physis”. Patients with more than 3 years of growth potential before maturity had better and faster outcomes. The severity of the deformity affected the rate of correction, which is further influenced by physis treated, femurs faster than tibias and hence a general observation that valgus deformities tend to correct faster than varus deformities.
Recommendations
Future studies are needed to assess TBP in correcting frontal plane deformities, such as flexion contractures. The presence of new designs in the market such as hinged plates needs to be compared to TBP, to check for and significant differences in treating such deformities in general.
Ethical approval
IRB approval granted from King Fahad Medical City, Riyadh, Saudi Arabia, Ethical Committee IRB Log No. 20-231E.
Declaration of patient consent
The authors certify that they have obtained all appropriate patient consent forms. In the form the patient(s) has/have given his/her/their consent for his/her/their images and other clinical information to be reported in the journal. The patients understand that their names and initials will not be published and due efforts will be made to conceal their identity, but anonymity cannot be guaranteed.
Acknowledgment
The authors would like to thank Dr. Rana AL-Rasheed for helping with the drawings.
Financial support and sponsorship
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Conflicts of interest
There are no conflicts of interest.
Authors' contribution
MIAG and AAA conceived and designed the study, conducted research, provided research materials, and collected and organized data. MA and AK analyzed and interpreted data. MIAG and KK wrote the initial and final draft of the article and provided logistic support. All authors have critically reviewed and approved the final draft and are responsible for the content and similarity index of the manuscript.
| 1. | Boero S, Michelis MB, Riganti S. Use of the eight-Plate for angular correction of knee deformities due to idiopathic and pathologic physis: Initiating treatment according to etiology. J Child Orthop 2011;5:209-16. [Google Scholar] |
| 2. | Phemister DB. Operative arrestment of longitudinal of bones in the treatment of deformities. J bone Joint Surg Am 1933;15:1-15. [Google Scholar] |
| 3. | Scott AC, Urquhart BA, Cain TE. Percutaneous vs. modified phemister epiphysiodesis of the lower extremity. Orthopedics 1996;19:857-61. [Google Scholar] |
| 4. | Bowen JR, Johnson WJ. Percutaneous epiphysiodesis. Clin Orthop Relat Res 1984;190:170-3. [Google Scholar] |
| 5. | Blount WP, Clarke GR. Control of bone growth by epiphyseal stapling; a preliminary report. J Bone Joint Surg Am 1949;31A:464-78. [Google Scholar] |
| 6. | Mielke CH, Stevens PM. Hemiepiphyseal stapling for knee deformities in children younger than 10 years: A preliminary report. J Pediatr Orthop 1996;16:423-9. [Google Scholar] |
| 7. | Métaizeau JP, Wong-Chung J, Bertrand H, Pasquier P. Percutaneous epiphysiodesis using transphyseal screws (PETS). J Pediatr Orthop 1998;18:363-9. [Google Scholar] |
| 8. | Khoury JG, Traverse JO, Mconnell S, Zeiders G, Sanders JO. Results of screw epiphysiodesis for the treatment limb length discrepancy and angular deformities. J Pediatr Orthop 2007;27:623-8. [Google Scholar] |
| 9. | Stevens PM. Guided growth for angular correction: A preliminary series using a tension band plate. J Pediatr Orthop 2007;27:253-9. [Google Scholar] |
| 10. | Burghardt RD, Herzenberg JE, Standard SC, Paley D. Temporary hemiepiphyseal arrest using a screw and plate device to treat knee and ankle deformities in children: A preliminary report. J Child Orthop 2008;2:187-97. [Google Scholar] |
| 11. | Burghardt RD, Herzenberg JE. Temporary hemiepiphysiodesis with the eight-Plate for angular deformities: Mid-term results. J Orthop Sci 2010;15:699-704. [Google Scholar] |
| 12. | Ballal MS, Bruce CE, Nayagam S. Correcting genu varum and genu valgum in children by guided growth: Temporary hemiepiphysiodesis using tension band plates. J Bone Joint Surg Br 2010;92:273-6. [Google Scholar] |
| 13. | Paley D. Principles of Deformity Correction. Berlin: Springer; 2002. [Google Scholar] |
| 14. | Fraser RK, Dickens DR, Cole WG. Medial physeal stapling for primary and secondary genu valgum in late childhood and adolescence. J Bone Joint Surg Br 1995;77:733-5. [Google Scholar] |
| 15. | Langenskiold A. Tibia vara; (osteochondrosis deformans tibiae); a survey of 23 cases. Acta Chir Scand 1952;103:1-22. [Google Scholar] |
| 16. | Schroerlucke S, Bertrand S, Clapp J, Bundy J, Gregg FO. Failure of Orthofix eight-Plate for the treatment of Blount disease. J Pediatr Orthop 2009;29:57-60. [Google Scholar] |
| 17. | Stevens PM, Klatt JB. Guided growth for pathological physes: Radiographic improvement during realignment. J Pediatr Orthop 2008;28:632-9. [Google Scholar] |
| 18. | McIntosh AL, Hanson CM, Rathjen KE. Treatment of adolescent tibia vara with hemiepiphysiodesis: Risk factors for failure. J Bone Joint Surg Am 2009;91:2873-9. [Google Scholar] |
| 19. | Danino B, Rödl R, Herzenberg JE, Shabtai L, Grill F, Narayanan U, et al. Guided growth: Preliminary results of a multinational study of 967 physes in 537 patients. J Child Orthop 2018;12:91-6. [Google Scholar] |
Fulltext Views
1,921
PDF downloads
358





