Translate this page into:
Neck of femur fracture with an ipsilateral concomitant supracondylar fracture following a low-energy injury: An important clinical lesson
2 Department of Trauma and Orthopaedics, Walsall Manor Hospital, Walsall, WS2 9PS; Department of Orthopaedics, Queen Elizabeth Hospital, Birmingham, B15 2TH, UK
Corresponding Author:
Jamie Hind
Department of Trauma and Orthopaedics, Walsall Manor Hospital, Walsall, WS2 9PS
UK
Jamie.hind@nhs.net
| How to cite this article: Hind J, Balakumar B, Selzer G. Neck of femur fracture with an ipsilateral concomitant supracondylar fracture following a low-energy injury: An important clinical lesson. J Musculoskelet Surg Res 2021;5:121-123 |
Abstract
Due to advancing age, neck of femur fractures is becoming increasingly more common. As the population continues to age, the rate of hip fractures with other associated injuries is also increasing. This case report is of a patient with an ipsilateral concomitant fracture of the proximal and distal femur and we discuss the importance of accurate history, examination and radiological assessment is needed to ensure these injuries are not missed.
Introduction
Fractures of the femoral neck are becoming increasingly more common as the population continues to age. Similarly, distal supracondylar fractures are also becoming more prevalent. Ipsilateral fractures of the proximal and distal femur, however, remain a rarity. Such injuries are often the result of a high-energy mechanism and typically occur in young adults. We report a rare case where a low-energy mechanism resulted in a neck of femur fracture and an ipsilateral supracondylar femur fracture that was initially missed, and later diagnosed on the operating table. The aim of this report is to highlight the importance of a detailed history and examination patients with fragility fractures, to ensure concomitant injuries are not missed.
Case Report
A 74-year-old female was admitted to hospital following a fall from her wheelchair. She lived in sheltered accommodation, which provided a video recording of the fall. She fell forwards from her chair onto her knees and then onto her right side. She had previously fallen two weeks earlier. Her past medical history included type two diabetes, a hemorrhagic stroke and a myocardial infarction. On admission, she was confused and complaining of pain in her right hip. On examination, there was bruising over her right hip and a blister over her right calf. She was tender over her right hip and unable to straight leg raise on the right. A plain radiograph of the pelvis revealed a right intracapsular fracture of the femoral neck [Figure - 1], which was treated with a cemented right hip hemiarthroplasty; however, during the procedure the right knee was unstable. Intra-operative imaging of the right knee was requested, which revealed an associated supracondylar fracture of the ipsilateral femur that had been missed on initial assessment [Figure - 2]. Intraoperatively, it was decided to manage the supracondylar fracture as a second procedure at a later date, as consent was not made to manage other injuries. Postoperatively the patient was slow to recover. A radiograph was performed of the distal femur to review the exact fracture pattern [Figure - 3]. A discussion was held with the patient's relatives regarding the diagnosis of the supracondylar fracture and the treatment options were also discussed. As the patient was slow to recover, it was decided to manage the supracondylar fracture conservatively. Unfortunately, the patient's condition declined, and the patient passed away a few weeks later.
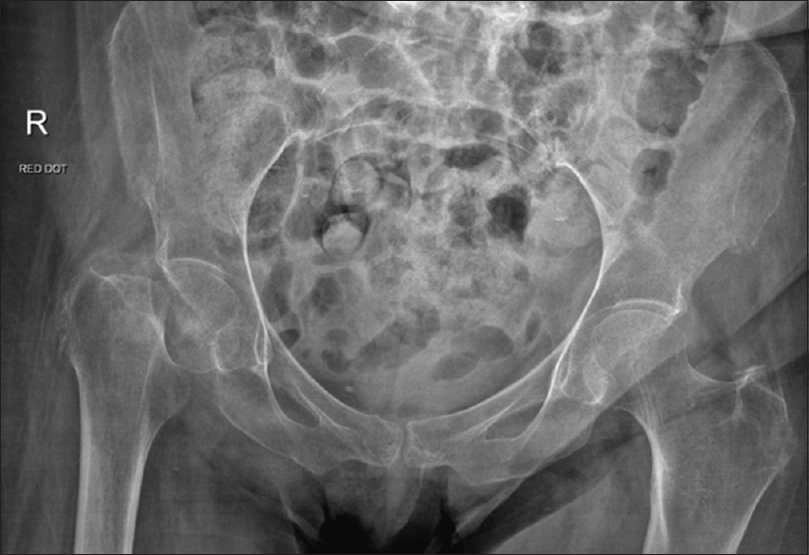 |
| Figure 1: Preoperative radiograph of pelvis revealing a right intracapsular neck of femur fracture |
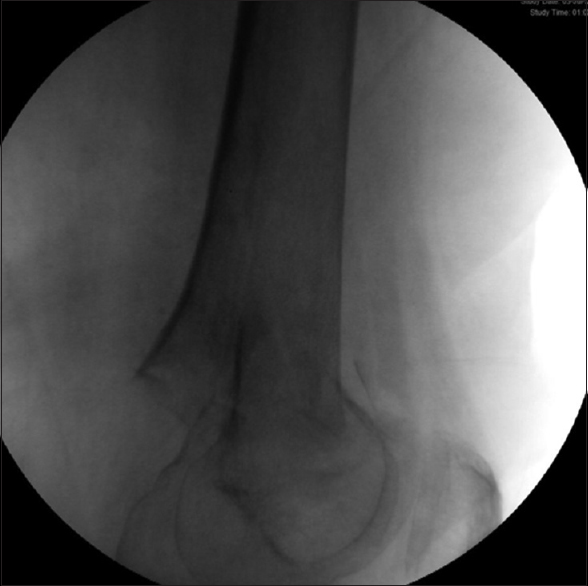 |
| Figure 2: Intraoperative imaging revealing a displaced ipsilateral distal femur fracture |
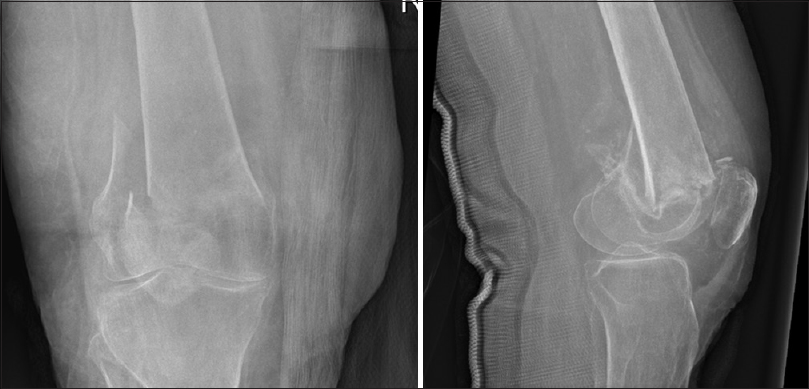 |
| Figure 3: Postoperative AP and lateral radiographs of the right knee. This demonstrates the fracture pattern of the distal femur |
Discussion
Neck of femur fractures are becoming increasingly prevalent as the population continues to age.[1] Most often, this type of fracture occurs in the elderly following a fall and results in pain, restricted range of movement and the inability to weight-bear. On examination, the affected limb may be shortened and externally rotated, and the patient is often tender over the hip and unable to actively or passively move the hip without eliciting pain. As a result, a full musculoskeletal examination distal to the femoral neck is often difficult and therefore, extra consideration should be taken to rule out an ipsilateral concomitant fracture distally. Ipsilateral concomitant fractures of the femur are rare injuries. When they do occur, it is typically the result of high-energy injuries in young adults.[2],[3],[4] Most ipsilateral concomitant fractures involve a fracture of the femoral shaft and an associated fracture of the femoral neck and this can be seen in approximately 2%–9% of femoral shaft fractures.[5],[6] Femoral shaft fractures with an associated fracture of the distal femur are less common, occurring in approximately 3%–4% of femoral shaft fractures.[7] Neck of femur fractures with an associated fracture of the distal femur are likely to be even less common, however, there is a lack of evidence on the prevalence of this fracture pattern to support this. Whilst these fracture patterns are rare, they are all typically a consequence of high-energy injuries. After conducting a literature search, we could only find one paper that analyzed neck of femur fractures with an ipsilateral distal femoral fracture.[8] This paper identified 15 cases of hip fractures with an associated distal femur fracture and the mechanism of injury in each case was high energy, either from a motorcycle or a car accident. This report is, therefore, a rare example of how these injuries can occur following low-energy trauma. It is likely that the patient sustained the femoral neck fracture and the supracondylar fracture simultaneously from the initial impact with the floor when falling from the chair onto her knees; however, it may be that the fractures occurred separately. One may have occurred when falling from her chair to her knees and the other when she fell from her knees onto her side. Alternatively, one may have occurred from either falling onto her knees or onto her side and the other from the fall the patient had 2 weeks previously. Regardless, it should be acknowledged that this low-energy mechanism resulted in a fracture pattern, which typically occurs following high-energy mechanisms, due to weakened osteoporotic bone. As well as appreciating the fracture pattern following this low impact mechanism, we must also address the reasons as to why the distal femur fracture was missed on initial assessment. The failure to diagnose an ipsilateral concomitant fracture of the femur on initial assessment is not universal to this case. It has been reported that 19%–50% of femoral neck fractures are misdiagnosed or overlooked at the initial presentation in patients with an Ipsilateral femoral shaft and femoral neck fracture.[9],[10] This is significant as the added knowledge of an associated fracture influences the treatment options for the patient. In order to reduce the risk of misdiagnosing an ipsilateral fracture of the femur, it is important to ensure that a thorough examination and a re-examination are performed. This may be difficult and therefore, it is also important to have a low threshold for requesting plain radiographs where the patient reports pain on palpation or when pain elsewhere prevents the admitting doctor from confidently ruling out other injuries and ensuring that radiographs includes the joint above and below the injury.
Summary
The increasing age of the population is resulting in increased pathological fractures, particularly of the proximal femur. Other fractures are also becoming increasingly common and it is not uncommon for concomitant fractures to occur. Falls on to the lower limb may result in ipsilateral concomitant fractures of the femur and it is important to identify these injuries and manage them accordingly.
Declaration of patient consent and the Ethical approval
The authors certify that they have obtained all appropriate patient consent forms. In the form, the patient has given her consent for her images and other clinical information to be reported in the journal. The patient understands that her name and initials will not be published and due efforts will be made to conceal identity, but anonymity cannot be guaranteed. Written consent was obtained.
Financial support and sponsorship
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Conflicts of interest
There are no conflicts of interest.
Authors' contributors
JH reviewed the case notes, documented the history of the patient and wrote the main bulk of the paper. BB Helped with writing the discussion of the paper and the literature review. The patient was admitted under GS care and identified this to be an important learning point that deserved publication. He requested the images and reviewed the final paper. All authors have critically reviewed and approved the final draft and are responsible for the manuscript's content and similarity index.
| 1. | Bunning T, Dickinson R, Fagan E, Inman D, Johansen A, Judge A, et al. National Hip Fracture Database (NHFD) Annual Report 2018. R Coll Physicians Lond UK 2017. [Google Scholar] |
| 2. | Barei DP, Schildhauer TA, Nork SE. Noncontiguous fractures of the femoral neck, femoral shaft, and distal femur. J Trauma 2003;55:80-6. [Google Scholar] |
| 3. | Alho A. Concurrent ipsilateral fractures of the hip and femoral shaft: A meta-analysis of 659 cases. Acta Orthop Scand 1996;67:19-28. [Google Scholar] |
| 4. | Swiontkowski MF. Ipsilateral femoral shaft and hip fractures. Orthop Clin North Am 1987;18:73-84. [Google Scholar] |
| 5. | Ostrum RF, Tornetta P 3rd, Watson JT, Christiano A, Vafek E. Ipsilateral proximal femur and shaft fractures treated with hip screws and a reamed retrograde intramedullary nail. Clin Orthop Relat Res 2014;472:2751-8. [Google Scholar] |
| 6. | Tsarouhas A, Hantes ME, Karachalios T, Bargiotas K, Malizos KN. Reconstruction nailing for ipsilateral femoral neck and shaft fractures. Strategies Trauma Limb Reconstr 2011;6:69-75. [Google Scholar] |
| 7. | Wood EG, Savoie FH, vander Griend RA. Treatment of ipsilateral fractures of the distal femur and femoral shaft. J Orthop Trauma 1991;5:177-83. [Google Scholar] |
| 8. | Chen CM, Chiu FY, Lo WH, Chuang TY. Ipsilateral hip and distal femoral fractures. Injury 2000;31:147-51. [Google Scholar] |
| 9. | Tornetta P 3rd, Kain MS, Creevy WR. Diagnosis of femoral neck fractures in patients with a femoral shaft fracture. Improvement with a standard protocol. J Bone Joint Surg Am 2007;89:39-43. [Google Scholar] |
| 10. | Labza S, Fassola I, Kunz B, Ertel W, Krasnici S. Delayed recognition of an ipsilateral femoral neck and shaft fracture leading to preventable subsequent complications: A case report. Patient Saf Surg 2017;11:20. [Google Scholar] |
Fulltext Views
1,332
PDF downloads
368





