Translate this page into:
Saudi orthopedic society guidelines for treating patients with bone and soft-tissue tumors during the COVID-19 pandemic
2 Department of Orthopeadic, Dr. Soliman Fakeeh Hospital, Jeddah, Saudi Arabia
3 Department of Orthopeadic, Prince Sultan Military Medical City, Riyadh, Saudi Arabia
4 King Saud Bin Abdulaziz University for Health Science, Riyadh, Saudi Arabia
5 ALRazi Hospital, Kuwait City, Kuwait
6 Department of Orthopeadic, King Faisel Specialist Hospital and Research Center, Riyadh, Saudi Arabia
7 Department of Reconstructive Orthopedic Surgery, King Fahad Medical City, Riyadh, Saudi Arabia
8 Department of Orthopaedic, King Saud University Hospital, Riyadh, Saudi Arabia
9 Department of Surgery, King Abdulaziz Medical City, Jeddah, Saudi Arabia
10 Department of Orthopeadic, King Abdulaziz University Hospital, Jeddah, Saudi Arabia
11 Department of Orthopedic Surgery, King Fahad Specialist Hospital, Dammam, Saudi Arabia
12 Department of Surgical Specialties, Johns Hopkins Aramco Healthcare Hospital, Dhahran, Saudi Arabia
13 Department of Orthopedic Surgery, Asir Central Hospital, Abha, Saudi Arabia
14 Department of Orthopedic Surgery, King Fahad Hospital, Medina, Saudi Arabia
15 Department of Orthopedic, King Abdulla Medical City, Makkah, Saudi Arabia
Corresponding Author:
Wazzan S Al Juhani
King Abdulaziz Medical City, King Abdullah Research Center, King Saud Bin Abdulaziz University for Health Science, Riyadh
Saudi Arabia
dr_wazzan@hotmail.com
| How to cite this article: Al Juhani WS, Al Sobeai MA, Alhamdan AA, Bobseit AH, Alanzi AM, Alqaseer AM, Edrees SO, Al Ghamdi A, Shaheen MF, Pant R, Alsulaimani SA, Al Shaya OS, Swan HM, Khan MA, Alshaygy IS, Alyami AH, Reda BR, Alabsi EJ, Alyamani MA, Alhifzi ZS, Almoftery IO, AL Arabi RM, AL Tayeb M, ALsayegh FF, Khan AM. Saudi orthopedic society guidelines for treating patients with bone and soft-tissue tumors during the COVID-19 pandemic. J Musculoskelet Surg Res 2021;5:10-14 |
Abstract
Objectives: The corona virus disease 2019 (COVID-19) pandemic has had a global effect and the Saudi Government has reacted aggressively to control the disease. Cancer patients are more susceptible to disease due to reduced immunity and are at higher risk of developing severe disease. In this article, we discuss the recommendations on slowing down the spread and easing the severity of COVID-19 in such patients. Methods: We have outlined guidelines and recommendations to be followed by orthopedic oncology centers in Saudi Arabia. These have been distributed to the Saudi Orthopedic Association-Oncology Chapter (SOA-OC) members for suggestions and recommendations. Results: A review of the literature was performed by searching for articles discussing COVID-19 measures related to cancer patients or patients undergoing surgical interventions during the pandemic. The authors discussed the recommendations and algorithmic pathways that were created to be implemented in orthopedic oncology centers around the country. Recommendations were reviewed by the SOA-OC members, who reached an agreement on application and publication. These recommendations focused on orthopedic cancer patient protection during clinical visits, inpatient, and surgical interventions. In addition, we discussed the recommendations for staff protection, including minimizing patient contact and continuing medical education during the pandemic. Conclusion: The reported algorithms and recommendations could help orthopedic oncology centers protect both their patients and staff from COVID-19 infection. These measures are highly recommended for continuing the treatment offered to orthopedic oncology patients, regardless of their infection status with COVID-19 during the pandemic.
Introduction
The coronavirus disease 2019 (COVID-19) pandemic presented a significant challenge to health-care systems globally. The Saudi government took rapid and unprecedented precautionary measures to limit this disease's explosive spread.[1],[2] Nevertheless, severe acute respiratory syndrome-coronavirus 2 (SARS-CoV-2) had infected almost 360,000 patients in Saudi Arabia by early December 2020.[3] This, in turn, jeopardized the ability of the health-care service to provide the required medical care for COVID-19 and non-COVID-19 patients. Cancer patients are more susceptible to infection than individuals without cancer because of the systemic immunosuppressive state caused by the malignancy and anticancer treatments. Moreover, they were observed to have a higher risk of severe events when infected with SARS-CoV-2.[4] Therefore, the guidelines in this article were formulated to reduce the unnecessary burden on the health-care system and the unnecessary risk of COVID-19 exposure to those already immunocompromised with bone and soft-tissue tumors. The Italian surgical oncology group has recently published their recommendations for treating oncology patients during the different phases of the pandemic.[5] However, no similar guidelines or recommendations are found in the literature for orthopedic oncology patients.
Methods
The authors reviewed the literature looking for updated international recommendations for COVID-19 management in different countries worldwide. In addition, national recommendations from the Saudi Ministry of Health in the form of daily reports and suggestions were scrutinized to develop a list of recommendations to be followed by oncology centers dealing with musculoskeletal cancer, including sarcoma and metastatic bone disease. The recommendation list was distributed to all orthopedic oncologists in Saudi Arabia for further discussion and validation before finalizing and proposing for publication.
The first six authors developed the initial draft of the guidelines after frequent online meetings. This process was followed by distributing the draft to all members of the Saudi Orthopedic Association, Oncology-Chapter. Comments were discussed through a controlled online social group. Comments regarding the feasibility of applications of the recommendations, when to do the swabs and other tests, in addition to comments related to virtual patient visits and clinics, were well taken and discussed. Voting was done to finalize opposing opinions and reach an overall agreement on algorithms and recommendations. These recommendations were feasible in all national oncology centers.
Results and Discussion
Surgical interventions
Based on the time from injury to intervention, an orthopedic surgery can be classified into priority A (emergency surgery within 24 h), priority B (urgent surgery within 48 h), priority C (expedited surgery within 2 weeks), priority D (short-term delayed, within 3 months), and priority E (long-term delayed, >3 months).[6] As recently published, individuals with more comorbidities were reported to be predisposed to worse clinical outcomes if infected by COVID-19. These comorbidities include those with increased age, diabetes, undergoing general anesthesia, and chronic obstructive pulmonary disease.[7] Hence, pre-operative optimization and clearance are important. The availability of resources such as personal protective equipment (PPE), intensive care unit (ICU) beds, and ventilators should be ensured and be ready for use if needed, as surgery carries a high risk of COVID-19 to the care providers and patients.[8]
A significant percentage of COVID-19 patients are clinically asymptomatic or show only mild symptoms. It is known by now that asymptomatic patients actively shed the virus unknowingly.[9] When a decision for surgical intervention has been made, the patient should always be assumed to be a virus carrier. A polymerase chain reaction (PCR) test should be conducted 24 h preoperatively. The patient should be isolated in his/her room,[10] and he/she should wear a face mask at all times.
In China, a multi-center study evaluated 34 patients who were in the incubation period of COVID-19 and underwent elective orthopedic surgery unintentionally without anyone knowing they were infected with COVID-19 preoperatively. Many of these patients had significant complications related to COVID-19 infection, with a 20.5% mortality rate and 44.1% rate of ICU admission postoperatively.[11] These complications and person-to-person contamination should ideally be avoided.
A compilation of current recommendations acquired from multiple sources internationally that can be implemented with continued improvements in testing is as follows:
- All patients and staff are required to wear masks during peri-operative contact, assuming that all patients could be positive for COVID-19[12],[13]
- All but emergent surgical patients should be tested preoperatively for COVID-19 according to the locally available resources (depending on the facility, real-time reverse transcriptase-PCR diagnostic panels can provide results in 4–6 h)[13],[14]
- Powered air-purifying respirators (PAPR) for all surgical staff and all patients with COVID-19 or N95 masks if no PAPRs are available.[15]
Surgeons and operating room (OR) staff should be wearing appropriate PPE, including an N95 respirator mask, face shield or goggles, gloves, and shoe covers. If possible, the surgery should be conducted in a negative-pressure, laminar flow room with an advanced particle filtration system.[16],[17],[18]
In general, we advise against operating on benign soft tissue masses in the extremity during a pandemic, as this incurs unnecessary utilization of hospital facilities, including hospital staff and hospital beds. Most importantly, this carries an unnecessary risk of occupying ICU beds that are high in demand. In addition, latent benign bone tumors (e.g., enchondroma, osteochondroma, nonossifying fibroma) should not be operated on unless there is a significant risk of pathological fracture and neurovascular compression. In patients with active benign bone tumors (e.g., aneurysmal bone cyst, simple bone cyst, and osteoid osteoma), we recommend exhausting the nonoperative options (if applicable) before operating, which should be a last resort. In aggressive benign tumors (e.g., giant cell tumor of the bone), we recommend treatment as required by the standard protocol.
Malignant bone and soft-tissue tumors are considered life-threatening conditions, and chemotherapy, radiotherapy, and the necessary operative interventions should not be delayed. Metastatic pathological fractures have been shown to worsen the prognosis of the disease, and hence, prevention and treatment should not be delayed, even during the current COVID-19 pandemic.[19]
Anesthetic procedures should be performed with caution owing to the potential spread of disease via infected droplets and aerosol. The highest risk of exposure occurs during the period when there is direct contact with respiratory droplets during airway management, primarily during intubation and extubation. Hence, a specific protection kit should be implemented for use during this procedure, and all intubations should be performed using a video laryngoscope to keep the head of the anesthesiologist away from the patient's mouth and to allow a faster procedure.[20]
The anesthesiologist and a dedicated nurse should dress in a filter room with a filtering facepiece 2 mask, a protective disposable gown that includes the neck and head, protective glasses, and disposable protectors for shoes. Health-care professionals not involved in the procedure should wait outside the operating room to reduce the contamination risk. Regional anesthesia, epidural, spinal, and supraclavicular anesthesia should be used as much as possible as these techniques can reduce the risk of COVID-19 transmission.[18]
Inpatient protocol
We recommend that the hospital length of stay (LOS) be reduced as much as possible. LOS has been reported to be associated with an increased risk of acquiring infection.[21] During the period of hospitalization, contact with the patient's companions should be prohibited or minimized, on a case-by-case basis, as assessed by the medical or administrative teams. Patients must be aware of the possible surgery complications, and they must contact the hospital if any complication occurs. The number of medical team members should be reduced during rounds, social distancing must be maintained, and they must be committed to health-care precautions. Daily rounds should be divided among trainees to reduce the risk of exposure.
Adjuvant and neo-adjuvant therapies
Chemotherapy and radiation therapy, whether adjuvant or neo-adjuvant, are mainstays in managing bone tumors and soft-tissue sarcomas. International studies report that cancer patients are at increased risk of SARS-CoV-2 infection and poor outcomes.[4],[22] A cohort study by Liang et al. concluded that cancer patients are at higher risk of many severe adverse events (ICU admission, mechanical ventilation, and death). In general, the utilization of adjuvant/neoadjuvant therapy is a multidisciplinary team (MDT) decision. Therefore, for adapting adjuvant/neoadjuvant therapy, MDT meetings may be necessary to ensure an optimal outcome and minimize infection risk to patients and health-care workers.
Categorizing patients by treatment and weighing the risks and benefits is essential. Prioritization of adjuvant therapy over palliative care for individuals with a high survival rate should continue, while patients with low to no survival rate may be considered a low priority.[23] Terminally ill individuals should be referred to palliative care service and managed at home if possible.
Orthopedic oncology outpatient clinics
Outpatient visits are generally avoided for nonlife-threatening conditions such as benign tumors, and visits may be delayed for a minimum of 3 months. However, patients with a growing tumor that is worrying or a suspected malignancy should visit the clinic on their own or with one companion at the most,[22] [Figure - 1] and [Figure - 2] show an algorithm to be followed in orthopedic oncology clinics].
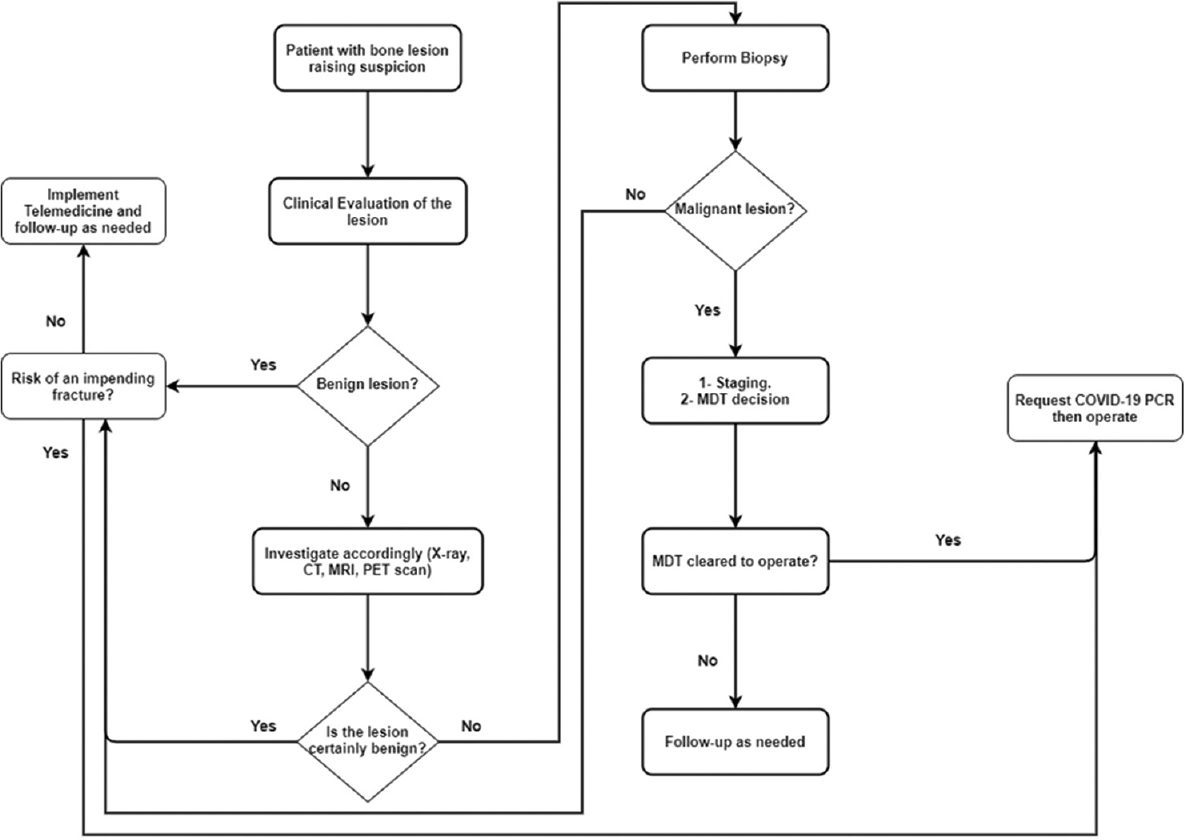 |
| Figure 1: Algorithmic pathway for patients with bone lesions. Management of benign lesions is conservative till the COVID-19 pandemic is over unless a pending fracture is identified. Malignant lesions are managed acutely with a multidisciplinary approach after COVID-19 surveillance |
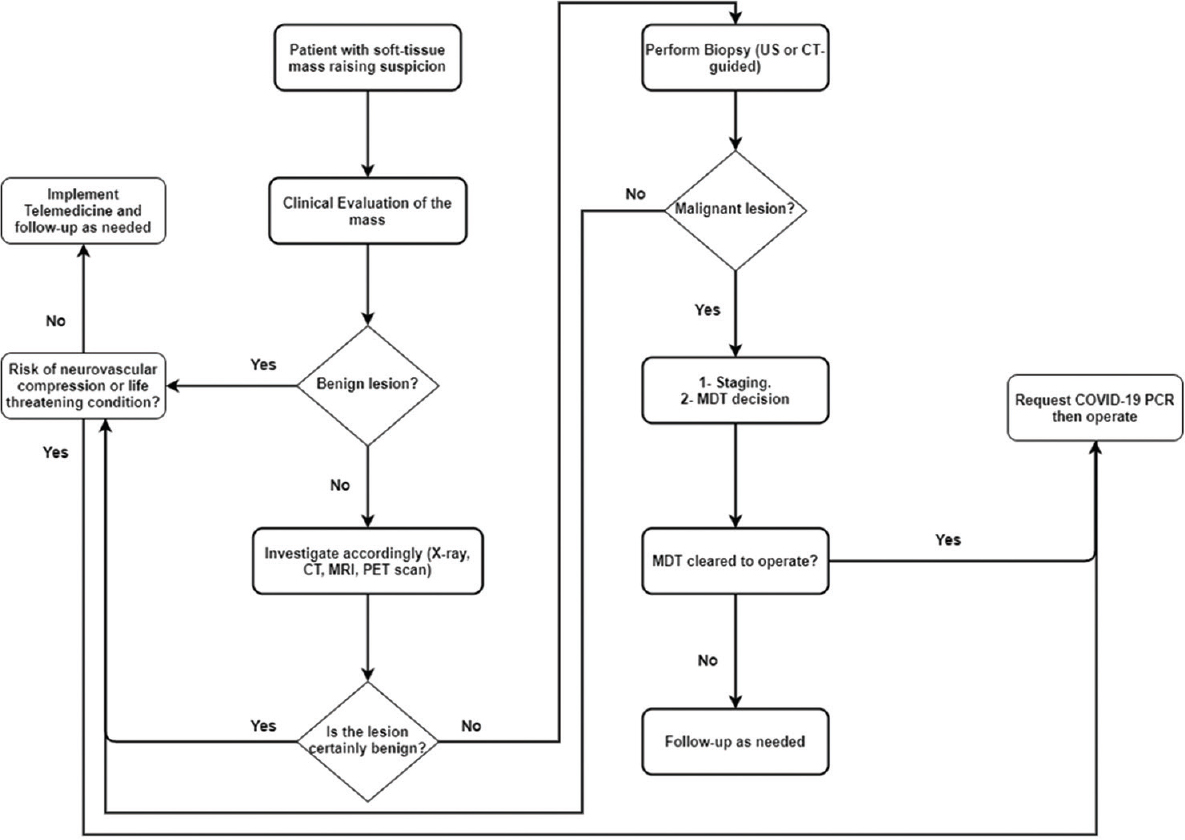 |
| Figure 2: Algorithmic pathway for patients with soft-tissue lesions. Management of benign lesions is conservative till the COVID-19 pandemic is over unless risking life or neurovascular structures. Malignant lesions are managed acutely with a multidisciplinary approach after COVID-19 surveillance |
If available, the use of virtual clinics is highly recommended. This is possible for patients that do not need physical visits and when their condition is not urgent. In addition, virtual sarcoma clinics should be created in far cities, especially during the complete or almost complete lockdown. This will allow closer observation in addition to the assessment of patients' needs. These include refill of medications, needs for further investigations/interventions, or solely need of physical visits.
Patients' triage should be done as follows: phone triaging in which history of contact and any history of fever, headache, and shortness of breath is enquired, screening checkpoint at the entrance of the clinic for both patients and health-care workers, checking individual temperatures by a thermal scanner or touchless thermometer, and hand hygiene with sanitizers. PPEs should be appropriately utilized, and no more than one companion should be allowed to enter the clinic with the patient.
If there is a history suggestive of a COVID-19 infection, the patient should go to a flu clinic for a COVID-19 PCR. Further follow-up visits are canceled until symptoms resolve, and any further tests are negative. However, patients whose tests are not suspicious should return to the clinic and maintain health precautions such as social distancing and masks.[24] Patient seats at the clinic should respect the safe distance, and everybody should have proper PPEs.
All waiting list cases should be re-organized based on the disease priority and available resources. Postoperatively, patients with malignancies should be contacted through telephone for follow-up. In cases of suspected complications, patients should be triaged as above. Cases that require immediate intervention are general exceptions after triage. Triage is of utmost importance to ensure that patients get the best care during this crisis.[22]
Residency, fellowship, and undergraduate training
Orthopedic oncology training for residents and fellows is an integral part of health systems and should be continued during this pandemic. PPE, hand sanitizers, and social distancing must be maintained. Online webinars must replace face-to-face lectures. Trainees must continue their learning through reading and online webinars. In addition, they can still continue learning while running the clinics and inpatient services, keeping in mind, they follow all the above recommendations. Program directors should address the deficiencies during the pandemic and try to compensate for them in future. Training for undergraduate medical students and interns should be continued with online classes and meetings. In-house education should be postponed until the pandemic is over.
Finally, the above recommendations should be followed during the pandemic in cancer centers to deal with oncology patients requiring medical and surgical interventions. In addition, they can be applied to other patients' populations with or without modifications. If any other pandemic happens in future, these recommendations and algorithms will be a good background to plan the management of health-care services and should be modified according to the nature of the organism and its mode of transmission.
Ethical approval
The authors confirm that this review had been prepared in accordance with COPE roles and regulations. Given the nature of the review, the IRB review was not required.
Financial support and sponsorship
This study did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Conflicts of interest
There are no conflicts of interest.
Authors' contributions
WSJ, MAS, AAH, AHB, AMA, and AMQ has conceived the idea and planned the project. AG contributed with resources to build the guidelines. Rest of the authors are involved in validation of the guidelines. All authors have critically reviewed and approved the final draft and are responsible for the manuscript's content and similarity index.
| 1. | Al-Tawfiq JA, Memish ZA. COVID-19 in the eastern mediterranean region and saudi arabia: Prevention and therapeutic strategies. Int J Antimicrob Agents 2020;55:105968. [Google Scholar] |
| 2. | Ebrahim SH, Memish ZA. Saudi Arabia's drastic measures to curb the COVID-19 outbreak: temporary suspension of the Umrah pilgrimage. J Travel Med. 2020;27. DOI: 10.1093/jtm/taaa029. [Google Scholar] |
| 3. | Weekly Epidemiological Update-15 December 2020; December, 2020. Available from: https://www.who.int/publications/m/item/weekly-epidemiological-update---15-december-2020. [Last accessed on 2021 Jan 14]. [Google Scholar] |
| 4. | Liang W, Guan W, Chen R, Wang W, Li J, Xu K, et al. Cancer patients in SARS-coV-2 infection: A nationwide analysis in China. Lancet Oncol 2020;21:335-7. [Google Scholar] |
| 5. | Cavaliere D, Parini D, Marano L, Cipriani F, Di Marzo F, Macrì A, et al. Surgical management of oncologic patient during and after the COVID-19 outbreak: practical recommendations from the Italian Society of Surgical Oncology. Updates Surg 2020; 2020:1-9. [Doi: 10.1007/s13304-020-00921-4]. [Google Scholar] |
| 6. | Massey PA, McClary K, Zhang AS, Savoie FH, Barton RS. Orthopaedic surgical selection and inpatient paradigms during the coronavirus (COVID-19) pandemic. J Am Acad Orthop Surg 2020;28:436-50. [Google Scholar] |
| 7. | Fan J, Liu X, Pan W, Douglas M, Bao S. Epidemiology of 2019 Novel Coronavirus Disease-19 in Gansu Province, China, 2020. Emerg Infect Dis 2020;26:1257-65. [Google Scholar] |
| 8. | Kaye K, Paprottka F, Escudero R, Casabona G, Montes J, Fakin R, et al. Elective, non-urgent procedures and aesthetic surgery in the wake of SARS-COVID-19: Considerations regarding safety, feasibility and impact on clinical management. Aesthetic Plast Surg 2020;44:1014-42. [Google Scholar] |
| 9. | Li C, Ji F, Wang L, Wang L, Hao J, Dai M, et al. Asymptomatic and human-to-human transmission of SARS-coV-2 in a 2-family cluster, Xuzhou, China. Emerg Infect Dis 2020;26:1626-8. [Google Scholar] |
| 10. | Al-Muharraqi MA. Testing recommendation for COVID-19 (SARS-coV-2) in patients planned for surgery - continuing the service and 'suppressing' the pandemic. Br J Oral Maxillofac Surg 2020;58:503-5. [Google Scholar] |
| 11. | Lei S, Jiang F, Su W, Chen C, Chen J, Mei W, et al. Clinical characteristics and outcomes of patients undergoing surgeries during the incubation period of COVID-19 infection. EClinicalMedicine 2020;21:100331. [Google Scholar] |
| 12. | Zucco L, Levy N, Ketchandji D, Aziz M, Ramachandran SK. Perioperative considerations for the 2019 novel coronavirus (COVID-19). Anesthesia Patient Safety Foundation 2020. Available from: https://www.apsf.org/article/an-update-on-the-perioperative-considerations-for-covid-19-severe-acute-respiratory-syndrome-coronavirus-2-sars-cov-2/. [Last Accessesed on 2020 Aug]. [Google Scholar] |
| 13. | Guo X, Wang J, Hu D, Wu L, Gu L, Wang Y, et al. Survey of COVID-19 disease among orthopaedic surgeons in Wuhan, people's republic of China. J Bone Joint Surg Am 2020;102:847-54. [Google Scholar] |
| 14. | Prada C, Chang Y, Poolman R, Johal H, Bhandari M. Best Practices for Surgeons. COVID-19 Evidence-Based Scoping Review. A Unifying Report of Global Recommendations. Orthoevidence; 2020. [Google Scholar] |
| 15. | Matos RI, Chung KK. DoD COVID-19 Practice Management Guide: Clinical Management of COVID-19. Defense Health Agency Falls Church United States; 2020. [Google Scholar] |
| 16. | Elizabeth Brindle M, Gawande A. Managing COVID-19 in surgical systems. Ann Surg 2020;272:e1-2. [Google Scholar] |
| 17. | Kim HJ, Ko JS, Kim TY. Recommendations for anesthesia in patients suspected of COVID-19 coronavirus infection. Korean J Anesthesiol 2020;73:89-91. [Google Scholar] |
| 18. | Brücher BL, Nigri G, Tinelli A, Lapeña JF, Espin-Basany E, Macri P, et al. COVID-19: Pandemic Surgery Guidance. 4Open 2020;3:1. [Google Scholar] |
| 19. | Saad F, Lipton A, Cook R, Chen YM, Smith M, Coleman R, et al. Pathologic fractures correlate with reduced survival in patients with malignant bone disease. Cancer 2007;110:1860-7. [Google Scholar] |
| 20. | Cook T, El-Boghdadly K, McGuire B, McNarry A, Patel A, Higgs A. Consensus guidelines for managing the airway in patients with COVID-19: Guidelines from the Difficult Airway Society, the Association of Anaesthetists the Intensive Care Society, the Faculty of Intensive Care Medicine and the Royal College of Anaesthetists. Anaesthesia 2020;75:785-99. [Google Scholar] |
| 21. | Hassan M, Tuckman Howard P, Patrick Robert H, Kountz David S, Kohn Jennifer L. Hospital length of stay and probability of acquiring infection. International Journal of Pharmaceutical and Healthcare Marketing. 2010;4:324-38.Available from: https://doi.org/10.1108/17506121011095182. DOI: 10.1108/17506121011095182. [Google Scholar] |
| 22. | Rajasekaran RB, Whitwell D, Cosker TD, Gibbons CL. Service delivery during the COVID-19 pandemic: Experience from the oxford bone tumour and soft tissue sarcoma unit. J Clin Orthop Trauma 2020;11 Suppl 4:S419-22. [Google Scholar] |
| 23. | Gulia A, Arora RS, Panda PK, Raja A, Tiwari A, Bakhshi S, et al. Adapting management of sarcomas in COVID-19: An evidence-based review. Indian J Orthop 2020:1-3. [Google Scholar] |
| 24. | Xiong Y, Chen L, Lin Z, Panayi AC, Mi B, Liu G, et al. Orthopaedic guidelines for the COVID-19 post-outbreak period: Experience from Wuhan, people's republic of China. J Bone Joint Surg Am 2020;102:e87. [Google Scholar] |
Fulltext Views
2,941
PDF downloads
667





