Translate this page into:
The role of processed nerve allograft in peripheral nerve surgery
Corresponding Author:
Amit Nijran
Queen Elizabeth Hospital Birmingham, Mindelsohn Way Edgbaston, B15 2GW Birmingham
UK
a_nijran@hotmail.com
| How to cite this article: Nijran A, Challoner TJ, Jordaan P, Power DM. The role of processed nerve allograft in peripheral nerve surgery. J Musculoskelet Surg Res 2019;3:110-115 |
Abstract
Objective: Peripheral nerve surgery involves the direct repair of peripheral nerves after trauma, reconstruction of nerve gaps and the management of painful nerve conditions such as end neuroma. There are a variety of situations where direct microsurgical repair is not possible or not the preferred option. Processed nerve allograft (PNA) offers a bespoke solution in the management of nerve gaps without the morbidity associated with autografts. Methods: A prospective database was populated for patients having nerve allograft implantation in the management of peripheral nerve injury. Results: Between July 2015 and November 2018 (40 months), 62 nerves in 45 patients were treated with AVANCE® PNA at the Birmingham Hand Centre at the Queen Elizabeth Hospital, Birmingham, UK. The mean age at implantation was 43 (range 16–77). Digital nerve reconstruction formed 50% of the total nerve repairs. Indications were 20 digital neuroma reconstructions, 13 neuromas after amputation, 20 traumatic injuries with nerve tissue loss, 8 delayed presentation after trauma, 3 contraindications to general anaesthesia, 4 insufficient autografts, 1 failed autograft and 3 tumour reconstructions. Conclusion: AVANCE® PNA is a useful tool in the reconstruction of peripheral nerve injury and the management of painful neuromas. An absolute indication is the management of painful neuromas in sensitised patients where avoidance of an additional site of neuropathic pain at a donor site is an important consideration. In digital neuroma management, there is good evidence to support use with equivalent efficacy to autologous sensory nerve grafts of a similar length.
Introduction
Peripheral nerve surgery encompasses the repair of primary nerve transection, the reconstruction of nerve gaps as well as the management of painful nerve conditions including end neuroma and neuroma-in-continuity. The gold standard for nerve repair is considered to be microsurgical suture with attention to restoring alignment and providing close approximation of the nerve ends without distortion of the fascicle architecture. Nerves, like other soft tissues such as skin exist in a pretensioned state. After transection, there is loss of this pretensioning or tension integrity (tensegrity) and subsequent retraction of the nerve ends. Sutures must overcome these forces; however, the strain that acts at the suture-nerve interface creates ischaemia and fibrosis,[1] which is a barrier to neural regeneration. Delay to surgery results in increasing modulus of elasticity of the nerve and higher forces acting at the repair site. Following a repair, the modulus reduces due to stress relaxation; however, the forces remain higher than for an acute nerve repair or for an intact nerve.[2] Detensioned primary nerve repair is now possible through creating a gap within a conduit, through using conduits to support a primary suture repair with remote sutures or using a conduit for sutureless nerve apposition with sutures only between the ends of the conduit and the epineurium remote from the site of injury. These latter two indications are essentially coaptation aids rather than conduits in the traditional sense and as such they may be more flexible devices without the need to be semi-rigid and resistant to compression as is necessary when unsupported neural regeneration is required over a distance. The aim of these innovations is to reduce the formation of scar at the repair site, improve the functional outcome and lower the rate of neuroma-in-continuity formation.
An alternative strategy for acute nerve detensioning is to interpose a nerve graft between the two ends at the site of injury to fill the tensegrity nerve gap, which is established through the positioning of a limb in full extension in the anatomical position after passive cycling of the injured area to allow normal physiological retraction and nerve excursion. The challenge in such reconstructions is balancing the risk of axon loss and neuroma formation at two coaptation sites versus the outcome of one neurorrhaphy with greater tension.[3],[4]
Delay to surgery also necessitates nerve end debridement to remove the scar and allow healthy fascicle apposition.[5] In this situation and in situ ations where there is loss of nerve tissue from trauma, the tension created by direct end-to-end repair is too high to support neural regeneration and an interposing nerve graft is the traditional method of reconstruction.[6],[7] For gaps >12 mm in a non-critical pure sensory nerve, a conduit may be used to provide a bridge across the gap. In all other situations where a gap must be reconstructed, a graft is needed. A reversed sensory autologous graft is usually selected for the reconstruction. Autografts provide a reliable physical micro-environment for axonal regeneration.[8],[9] The site of donor harvest is dictated by the diameter of the nerve at the repair site and the gap length. Larger recipient nerves require a cabling configuration of several strips of autologous donor graft to cover the nerve ends due to donor-recipient diameter mismatch. Donor sites in common use include the medial cutaneous nerve of the forearm and the lateral cutaneous nerve of the forearm in the upper limb and the sural nerve in the lower limb. In an adult, approximately 30 cm of donor sural nerve can be harvested from each leg. Donor-site sensory loss is acceptable; however, there are the added risks of surgery on the leg: general anaesthesia may be required when donor and recipient nerves are in different limbs, patients have two surgical sites (with risks of scarring, pain and infection) and there is a small risk of symptomatic neuroma formation at the harvest site estimated at between 6% and 8%.[8],[10],[11]
An alternative strategy is to use a nerve allograft to bridge the gap. AVANCE® processed nerve allograft (PNA) (AxoGen Inc. Alachua, Florida, USA) is derived from human nerve and is treated to provide an acellular and therefore immunologically inert, 3-dimensional endoneurial tube microstructure to scaffold axon regeneration. Neurotoxic chondroitin sulphate proteoglycans within the basement membrane are selectively degraded by chondroitinase to provide an environment that supports axon regeneration.[8],[10] Host Schwann cells must migrate into the graft to maintain nerve growth. The host must revascularise the graft, and therefore, the condition of the nerve ends and the surgical bed is important in determining the success of any graft. Allografts >5 mm in diameter vascularise less well and so the maximum diameter commercially available in AVANCE® allograft is 4–5 mm in diameter. The allograft is provided frozen in a range of diameters between 1 and 5 mm and lengths up to 70 mm. A number of clinical studies have supported their use in peripheral nerve surgery.[6],[12],[13]
Allografts offer a bespoke solution to managing a nerve gap. The length may be selected after adequate debridement and the graft length is not dictated by available graft. Single limb surgery facilitates regional anaesthesia rather than general anaesthesia enabling surgery to be safely completed in patients with major co-morbidities and reducing the risks of lower limb donor harvest surgery in patients with a history of vascular disease, diabetes or prior thromboembolic events. Surgical time is reduced, hospital stay is reduced and the risks of donor site morbidity are avoided. These compelling reasons for using an allograft as a default in nerve gap management must be weighed against the added cost and the limited evidence base for efficacy in long gaps and in mixed motor and sensory nerve gap reconstruction. PNA was introduced to our regional peripheral nerve injury service in the UK 3 years ago. There are absolute and relative indications for allograft utilisation. Patients are provided with written information regarding the allograft safety and efficacy in keeping with the National Institute for health and Care Excellence interventional procedural guidance (NICE IPG: 597)[14] released in November 2017. All allograft nerve repairs have prospective outcome data collection, and where consent is provided and inclusion criteria are met, data are shared with the international RANGER registry study for pooled outcome analysis.[8],[15]
Materials and Methods
Following the introduction of AVANCE® PNA (AxoGen Inc. Alachua, Florida, USA) to our unit in July 2015, a prospective database was populated for patients having nerve allograft implantation in the management of peripheral nerve injury. Patient demographics, details of the injury mechanism, injured nerve, injury site, gap length, size of allograft, indication for allograft, method of coaptation, clinical outcomes and complications are recorded. The indications for allograft utilisation were extracted and evaluated to establish absolute and relative indications for allograft implantation in our unit.
Results
The regional peripheral nerve injury service is based within the Birmingham Hand Centre at the Queen Elizabeth Hospital, Birmingham, UK. The hospital is part of the University Hospitals NHS Foundation Trust and receives civilian referrals from the region with a catchment population of approximately 2.5 million for hand trauma and 6 million for brachial plexus injuries. In addition, it is the Royal Centre for Defence Medicine receiving all UK-injured military personnel including those deployed overseas.
Between July 2015 and November 2018 (40 months), 62 nerves in 45 patients were treated with AVANCE® PNA in our unit. The mean age at implantation was 43 (range 16–77). The distribution by nerve type was 40 sensory (31 digital; 9 other upper limb), 3 motor and 19 mixed motor-sensory.
The indications for allograft use are listed in [Table - 1]. Four were for insufficient autograft available (3 were reconstructions using hybrid autologous and allograft; 1 was for a patient with bilateral sural harvest for a brachial plexus injury with a concomitant distal median nerve injury). Three of the lower limb and 4 of the upper limb long gap reconstruction cases had an adjunctive distal motor nerve transfer. There were 12 iatrogenic nerve injuries in this series.

Of the 31 digital nerve reconstructions, 28 were management of a gap and 3 were for proximal redirection of an end neuroma. In the 28 gap reconstructions (17 neuromas), 6 were for neuromas after previous repair, 2 for a neuroma-in-continuity from trauma and 9 for end neuroma from late presenting or missed injuries. The mean allograft length was 16.5 mm (range 10–40 mm) [Figure - 1].
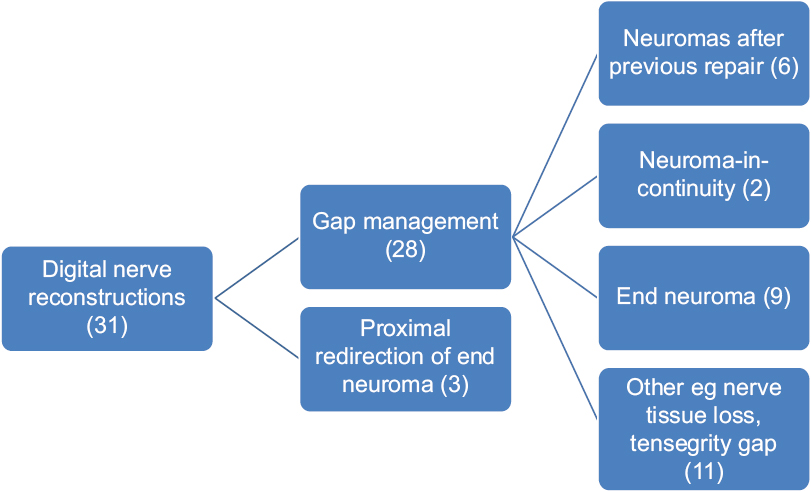 |
| Figure 1: Allograft use for digital nerve reconstruction |
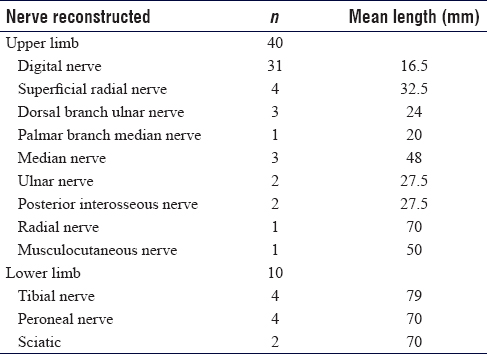
The anatomical distribution of the other sensory allograft reconstructions were 4 superficial radial nerves (mean 32.5 mm; range 25–40 mm), 1 palmar branch median nerve (20 mm), 3 dorsal cutaneous branch ulnar nerve (mean 24 mm; range 15–40 mm) and 1 superficial ulnar nerve (42 mm).
The motor nerves were 1 deep branch of the ulnar nerve (28 mm) and 2 posterior interosseous nerves (mean 27.5 mm; range 35–50 mm).
The mixed nerve reconstructions included 3 median nerves (mean 48 mm; range 30–65 mm), 1 musculocutaneous nerve (50 mm), 1 radial nerve (70 mm), 2 ulnar nerves (27.5 mm; range 25–30 mm), 1 C8 root (70 mm), 1 T1 root (70 mm), 3 common peroneal (mean 140 mm; range 70–170 mm), 1 proximal superficial peroneal (70 mm), 4 tibial (mean 79 mm; 45–120 mm) and 2 sciatic nerves (both 70 mm) [Table - 2].
Five nerves were treated with allograft as a 'graft to nowhere' for end neuromata following amputation: 3 digital and 1 sciatic (2 mm × 70 mm allografts – one for each common peroneal and tibial components). Rerouting was for direct intramuscular implantation in 3 and as a loop centrocentral graft in 2.
Three allograft reconstructions were for tumour reconstruction (2 were for reconstruction of nerve root gaps at C8 and T1 for pain management after sarcoma resection with a distal functional reconstruction with tendon transfers; 1 for reconstruction of a gap following resection of a recurrent neurofibroma in the median nerve).
Discussion
The indication for using allograft can be broadly reported as absolute or relative. Absolute indications were for reconstruction of painful neuromata in patients with neuropathic pain and sensitisation, graft to nowhere for painful end neuromata, insufficient donor nerve availability and reconstruction of gaps following tumour resection to prevent neuropathic pain with or without distal motor nerve transfer reconstruction. Relative indications included previous failed autologous grafting, late-presenting cases with large gaps where surgery is for pain management or prevention rather than functional recovery, replantation where the amputated part may not survive, gap management in a mixed nerve when distal motor nerve transfer is employed for critical functions, acute detensioning repairs in non-critical sensory nerves and patient choice. The indications are presented in [Table - 3].

PNAs have demonstrated superior clinical results compared to hollow conduits for the reconstruction of digital nerve gaps <25 mm.[15] Brooks et al. performed a multicentre retrospective review of PNA reconstruction and found PNAs provide a safe and effective reconstruction method for gaps between 5 and 50 mm. The outcomes compare favourably to autografts and are superior to collagen tube conduits.[8]
These findings were also supported in a retrospective review by Cho et al.[16] Both these studies utilised data from the RANGER registry, a large active international database of processed allograft repairs (AVANCE® Nerve Graft; AxoGen, Inc, Alachua, FL). Furthermore, in a non-randomised comparative study of 153 patients needing digital nerve repair comparing PNAs with tension-free neurorrhaphy, two-point discrimination was not significantly different between the two groups.[17] Failure rates for nerve grafting where there was no sensory recovery occurred in 5% of patients in a case series of 108 patients needing nerve repair.[8] The National Institute for Health and Care Excellence in the UK reviewed all evidence relating to the use of processed nerve grafts to repair peripheral nerve discontinuities in 2017 and found that although there is limited high-quality evidence (only one randomised study with insufficient data to be powered[7]), the safety and efficacy of PNAs is adequate to support their use for digital nerve repairs, providing standardised arrangements are in place for clinical governance, consent and audit.[14] Enhanced governance and outcome data collection should be in place for use in non-digital sensory reconstruction and mixed motor-sensory nerve reconstruction. It recommended that patients receive written guidance on nerve allograft before surgery.
In our practice, reimbursement is not sufficient to cover the additional cost of the nerve allograft despite reduced theatre, hospital and drug costs compared with autologous nerve graft harvest and gap reconstruction. As such, the main indication for AVANCE® processed nerve graft utilisation is in the management of symptomatic painful neuromas in patients exhibiting signs of sensitisation where the risk of creating an additional pain source at the site of autologous nerve harvest is significant and the function to be restored is noncritical. The main aim of surgery is pain resolution and not functional recovery, and in such a case, processed allograft is a reliable option. The typical scenario is a painful end neuroma or neuroma-in-continuity in a digital nerve or in a non-critical non-digital sensory peripheral nerve [Figure - 2] and [Figure - 3]. In cases with a painful end neuroma and poor-quality tissues, where there is no distal nerve stump or in cases of an end neuroma in an amputation stump, nerve allograft can be used as a graft to nowhere to reroute the nerve after neuroma resection to deeper and healthier tissues.
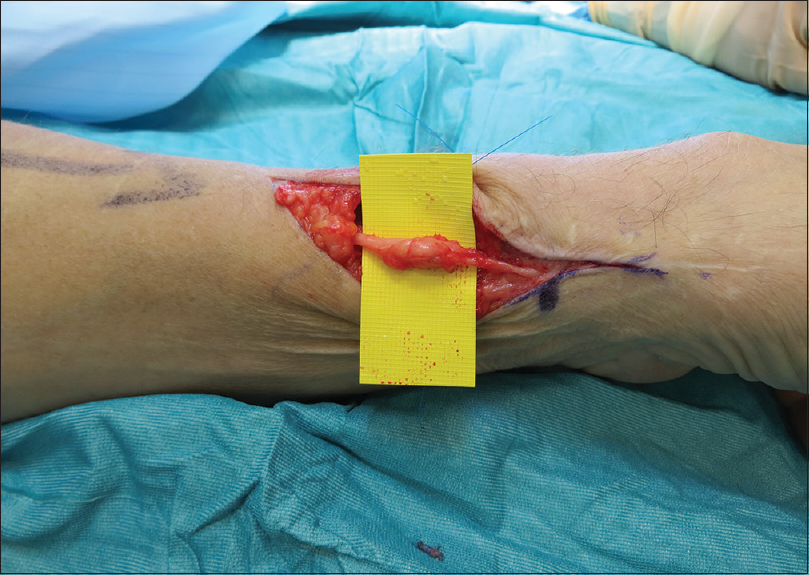 |
| Figure 2: Superficial radial nerve after repair with subsequent neuroma formation |
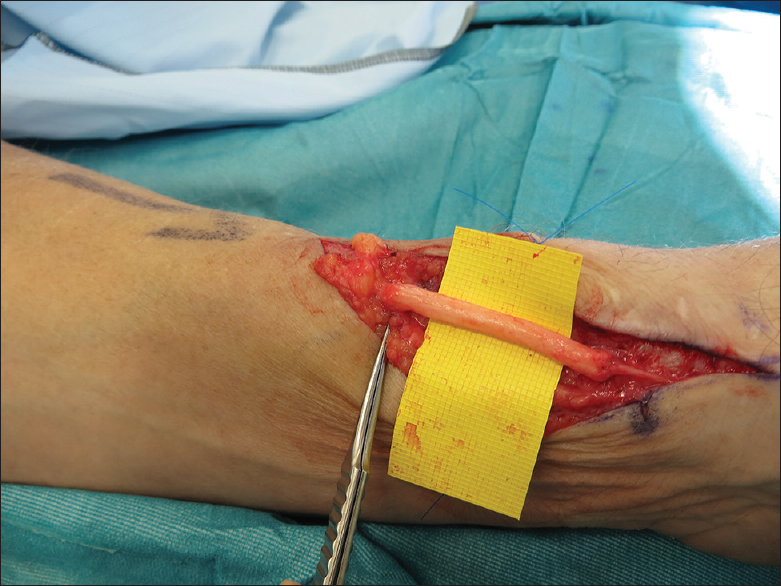 |
| Figure 3: Repair of the superficial radial nerve neuroma with a processed allograft reconstruction |
Additional absolute indications in our unit include insufficient autologous graft, after tumour resection and in proximal nerve injuries when a distal functional reconstruction with nerve or tendon transfers is performed.
In complex cases, there may be insufficient autologous nerve graft reconstruction of large gaps in multiple nerves. In our unit, we have used allograft in a patient with a high transfemoral and contralateral hemipelvic amputation, in a case with bilateral lower limb trauma with no sural nerves available, in a case where both sural nerves were harvested and supplemented by allograft and in a case where a previously failed autograft was salvaged with an allograft reconstruction.
Allograft can be used in conjunction with autologous nerves as a hybrid graft reconstruction where an allograft of smaller diameter than the nerve to be reconstructed is placed across the defect and one or two cables of autologous nerve graft are placed alongside it.
In rare cases of tumour resection with preoperative radiotherapy, when a nerve trunk must be sacrificed, nerve allograft provides an option to reconstruct the gap and reduce the risk of nerve pain. In a scarred bed following radiotherapy, any free non-vascularised nerve graft will not support reliable neural regeneration, and in such a case, we would undertake a functional distal reconstruction with tendon or nerve transfers and use the nerve allograft for an anatomical restoration of nerve trunk continuity.
The same approach can be adopted in late-presenting, proximal, large nerve gaps from nerve rupture or following resection of a neuroma-in-continuity. Distal motor nerve transfer may be the preferred functional reconstruction, and so, nerve allograft is utilised for anatomical restoration and gap management to provide a pathway for regenerating nerve fibres to reduce the impact of neuropathic pain from recurrent neuroma formation in scar.
The use of nerve allograft in other situations is a relative indication based on the current available evidence. PNA is an elegant solution for acute nerve reconstruction in the setting of digit replantation. The time saved from not having to harvest an autologous nerve is critical, and the allograft can be placed with radical debridement to healthy stumps, avoiding interval re-exploration and grafting at 6–12 weeks after successful replantation. In the case of a digit not surviving, no autologous nerve is lost, thereby minimising the morbidity of the patient to the amputated part [Figure - 4].
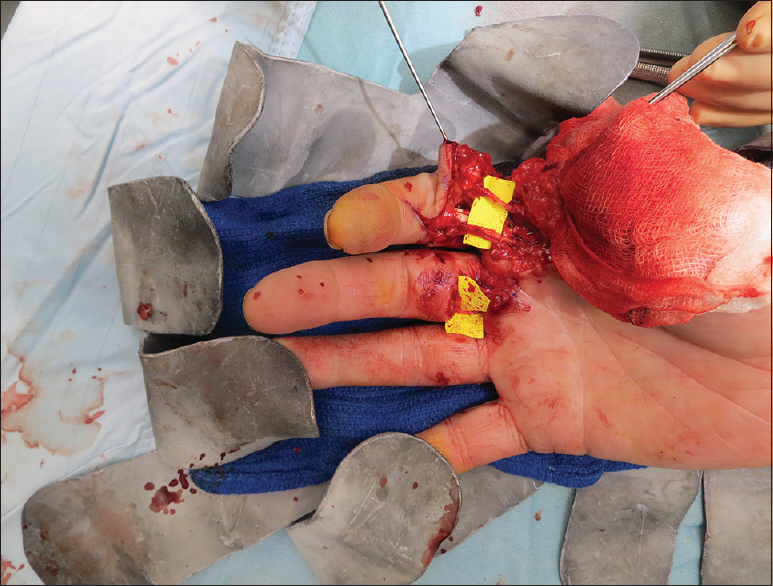 |
| Figure 4: A thumb replant and index finger revascularisation shows multiple processed nerve allografts for digital nerve reconstructions. Avoids later re-exploration and possible failed autografts |
In detensioning primary nerve repair in the hand, nerve allograft interposition to the tensegrity gap may allow early functional mobilisation without the need for protective immobilisation. There are no studies looking at this particular scenario, and so, this remains a relative indication, limited in our practice by the cost of the nerve allograft.
We have used nerve allograft in a patient with a flail chest and lung contusion that precluded general anaesthesia who required upper limb nerve reconstruction and time-critical local flap cover to exposed metalwork. An axillary block was used for anaesthesia and a double-cabled nerve allograft with stepped neurorrhaphies was used to reconstruct the sensory and motor components of the ulnar nerve in the distal forearm [Figure - 5].
 |
| Figure 5: Double-cabled nerve allografts with stepped neurorrhaphies used to reconstruct the sensory and motor components of the ulnar nerve in the distal forearm |
Patients are becoming aware of the option for nerve allograft in nerve gap management, and peripheral nerve surgeons must provide appropriate preoperative counselling regarding the evidence base and efficacy of nerve allograft in a particular indication. We have used nerve allograft to reconstruct a mixed nerve iatropathic injury in a patient who refused to allow general anaesthesia and autologous sural nerve harvesting. AVANCE® processed nerve graft was deemed an acceptable alternative and provided a good functional recovery albeit with a longer reinnervation time than would be anticipated for an autologous graft of the same length.
The evolving evidence base means that the potential indications for nerve allograft utilisation will expand. There is considerable heterogenecity between studies to date and limited data on medium to long-term follow-up.[14] It is not possible to perform a blinded study of nerve autograft versus allograft. Non-digital randomised studies are needed; however, the low incidence of injury and the inability to control the site of injury and the mechanism of trauma mean that recruitment would need large multicentre trials to recruit sufficient numbers of patients. The follow-up of mixed nerve studies also is longer than for digital nerve studies due to the longer reinnervation time. Ranger is an ongoing registry study collecting large patient datasets and therefore allowing analysis of subsets of patients and injured nerves, while maintaining statistical power. Interim analysis has demonstrated comparable functional recovery in sensory nerve gap reconstruction up to 50 mm.[8]
There are limitations to this study. First, it is a single-centre retrospective study and therefore has the inherent biases associated with retrospective studies. Furthermore, the unique structure of healthcare within the UK and the NHS and within our unit means the cost of the allograft is not offset by the reduced theatre time, drug and hospital costs. This may not be the same in other institutions or countries, and therefore, direct comparison to other settings is difficult.
Conclusion
AVANCE® PNA is a useful tool in the reconstruction of peripheral nerve injury and the management of painful neuromas. It offers a bespoke solution for gap management after nerve debridement, providing simple, quick and reproducible neurorrhaphy without donor morbidity. An absolute indication is the management of painful neuromas in sensitised patients where avoidance of an additional site of neuropathic pain at a donor site is an important consideration. In digital neuroma management, there is good evidence to support use with equivalent efficacy to autologous sensory nerve grafts of a similar length. The evidence for use in sensory nerve reconstruction at other sites and for reconstruction of mixed motor and sensory nerves is more limited, but the evidence base continues to develop.
Ethical consideration
Informed consent for publication of all photos was obtained.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
Authors' contributions
AN wrote initial and final draft, involved in planning, collating, analysing and interpretation, TJC analysis of work, revising it critically for important intellectual content, PJ provided research materials and data, DMP design and conception of article, research data, final draft. All authors have critically reviewed and approved the final draft and are responsible for the content and similarity index of the manuscript.
| 1. | Mackinnon SE, Dellon AL. Surgery of the Peripheral Nerve. New York: Theime Medical Publishers; 1988. [Google Scholar] |
| 2. | Toby EB, Rotramel J, Jayaraman G, Struthers A. Changes in the stress relaxation properties of peripheral nerves after transection. J Hand Surg Am 1999;24:694-9. [Google Scholar] |
| 3. | Hentz VR, Rosen JM, Xiao SJ, McGill KC, Abraham G. The nerve gap dilemma: A comparison of nerves repaired end to end under tension with nerve grafts in a primate model. J Hand Surg Am 1993;18:417-25. [Google Scholar] |
| 4. | Wall EJ, Kwan MK, Rydevik BL, Woo SL, Garfin SR. Stress relaxation of a peripheral nerve. J Hand Surg Am 1991;16:859-63. [Google Scholar] |
| 5. | Madison RD, Archibald SJ, Lacin R, Krarup C. Factors contributing to preferential motor reinnervation in the primate peripheral nervous system. J Neurosci 1999;19:11007-16. [Google Scholar] |
| 6. | Whitlock EL, Tuffaha SH, Luciano JP, Yan Y, Hunter DA, Magill CK, et al. Processed allografts and type I collagen conduits for repair of peripheral nerve gaps. Muscle Nerve 2009;39:787-99. [Google Scholar] |
| 7. | Means KR Jr., Rinker BD, Higgins JP, Payne SH Jr., Merrell GA, Wilgis EF, et al. Amulticenter, prospective, randomized, pilot study of outcomes for digital nerve repair in the hand using hollow conduit compared with processed allograft nerve. Hand (N Y) 2016;11:144-51. [Google Scholar] |
| 8. | Brooks DN, Weber RV, Chao JD, Rinker BD, Zoldos J, Robichaux MR, et al. Processed nerve allografts for peripheral nerve reconstruction: A multicenter study of utilization and outcomes in sensory, mixed, and motor nerve reconstructions. Microsurgery 2012;32:1-14. [Google Scholar] |
| 9. | Lee SK, Wolfe SW. Peripheral nerve injury and repair. J Am Acad Orthop Surg 2000;8:243-52. [Google Scholar] |
| 10. | Taras JS, Amin N, Patel N, McCabe LA. Allograft reconstruction for digital nerve loss. J Hand Surg Am 2013;38:1965-71. [Google Scholar] |
| 11. | Ortigüela ME, Wood MB, Cahill DR. Anatomy of the sural nerve complex. J Hand Surg Am 1987;12:1119-23. [Google Scholar] |
| 12. | Grahan JB, Neubauer D, Quing Shan X, Muir D. Chondroitinase-treated, decellurised nerve allograft compares favourably to the cellular isograft in rat peripheral nerve repair. J Neurodegener Regen 2009;2:162-70. [Google Scholar] |
| 13. | Karabekmez FE, Duymaz A, Moran SL. Early clinical outcomes with the use of decellularized nerve allograft for repair of sensory defects within the hand. Hand (N Y) 2009;4:245-9. [Google Scholar] |
| 14. | NICE. Processed Nerve Allografts to Repair Peripheral Nerve Discontinuities. Interventioanl Procedures Guidance. Available from: http://www.nice.org.uk/guidance/ipg597. [Last accessed on 2017 Nov 22]. [Google Scholar] |
| 15. | Rinker B, Zoldos J, Weber RV, Ko J, Thayer W, Greenberg J, et al. Use of processed nerve allografts to repair nerve injuries greater than 25 mm in the hand. Ann Plast Surg 2017;78:S292-5. [Google Scholar] |
| 16. | Cho MS, Rinker BD, Weber RV, Chao JD, Ingari JV, Brooks D, et al. Functional outcome following nerve repair in the upper extremity using processed nerve allograft. J Hand Surg Am 2012;37:2340-9. [Google Scholar] |
| 17. | He B, Zhu Q, Chai Y, Ding X, Tang J, Gu L, et al. Safety and efficacy evaluation of a human acellular nerve graft as a digital nerve scaffold: A prospective, multicentre controlled clinical trial. J Tissue Eng Regen Med 2015;9:286-95. [Google Scholar] |
Fulltext Views
3,833
PDF downloads
527





